Professional Documents
Culture Documents
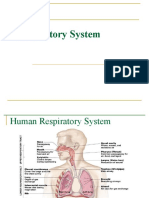
Respiratory System Overview and Gas Exchange
Uploaded by
Nabila0 ratings0% found this document useful (0 votes)
23 views64 pagesThe respiratory system functions to oxygenate cells and remove carbon dioxide through two main processes: external respiration which is the exchange of gases between the lungs and blood, and internal respiration which is the exchange of gases between blood and tissues at the cellular level. The main organs involved include the nasal passages, pharynx, larynx, trachea, bronchi, lungs, and the blood and heart which transport gases. Oxygen and carbon dioxide move between the alveoli, capillaries, and tissues down partial pressure gradients, and changes in thoracic pressure and volume drive the processes of inhalation and exhalation.
Original Description:
kulpak upn
Original Title
Kulpak UPN - Fisiologi Respirasi 1
Copyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe respiratory system functions to oxygenate cells and remove carbon dioxide through two main processes: external respiration which is the exchange of gases between the lungs and blood, and internal respiration which is the exchange of gases between blood and tissues at the cellular level. The main organs involved include the nasal passages, pharynx, larynx, trachea, bronchi, lungs, and the blood and heart which transport gases. Oxygen and carbon dioxide move between the alveoli, capillaries, and tissues down partial pressure gradients, and changes in thoracic pressure and volume drive the processes of inhalation and exhalation.
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
23 views64 pagesRespiratory System Overview and Gas Exchange
Uploaded by
NabilaThe respiratory system functions to oxygenate cells and remove carbon dioxide through two main processes: external respiration which is the exchange of gases between the lungs and blood, and internal respiration which is the exchange of gases between blood and tissues at the cellular level. The main organs involved include the nasal passages, pharynx, larynx, trachea, bronchi, lungs, and the blood and heart which transport gases. Oxygen and carbon dioxide move between the alveoli, capillaries, and tissues down partial pressure gradients, and changes in thoracic pressure and volume drive the processes of inhalation and exhalation.
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You are on page 1of 64
Functional Human Physiology
The Respiratory System
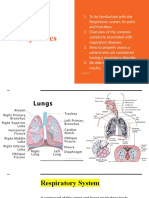
Overview of Respiratory Function
Respiration = the process of gas exchange
Two levels of respiration:
Internal respiration (cellular respiration)
The use of O
2
with mitochondria to generate ATP
by oxidative phosphorylation
CO
2
is the waste product
External respiration (ventilation)
The exchange of O
2
and CO
2
between the
atmosphere and body tissues
Internal respiration (cellular
respiration)
Involves gas exchange between capillaries and
body tissues cells
Tissue cells continuously use O
2
and produce CO
2
during
metabolism
Partial pressure (P)
The PO
2
is always higher in arterial blood than in the
tissues
The PCO
2
is always higher in the tissues than in arterial
blood
O
2
and CO
2
move down their partial pressure
gradients
O
2
moves out of the capillary into the tissues
CO
2
moves out of the tissues into the capillary
External respiration (ventilation)
4 Processes:
Pulmonary Ventilation
Movement of air into the lungs (inspiration) and
out of the lungs (expiration)
Exchange of O
2
and CO
2
between lung air
spaces and blood
Transportation of O
2
and CO
2
between the
lungs and body tissues
Exchange of O
2
and CO
2
between the blood
and tissues
Overview of Pulmonary Circulation
Deoxygenated blood
Under resting conditions, 5 liters of deoxygenated
blood are pumped to the lungs each minute from
the right ventricle
CO
2
blood concentration is higher than O
2
blood
concentration in:
Systemic veins
Right atrium
Right ventricle
Pulmonary arteries
Overview of Pulmonary Circulation
Oxygenated blood
Transported from the pulmonary capillaries pulmonary
veins left atrium left ventricle aorta systemic
arterial circulation
O
2
blood concentration is higher than CO
2
blood
concentration in:
Alveoli
Pulmonary capillaries
Pulmonary veins
Left atrium
Left ventricle
Systemic arteries
The Respiratory System
Cells continually use
O2 & release CO2
Respiratory system
designed for gas
exchange
Cardiovascular
system transports
gases in blood
Failure of either
system
rapid cell death from
O2 starvation
Nose -- Internal Structures
two nasal cavities with bony
outgrowths = nasal conchae (superior,
middle, inferior)
nasal cavities separated by nasal
septum and nasal bone
lined with: pseudostratified ciliated
epithelial cells - mucus production
also are receptors for odors -lead to
nerves -> brain (smell)
lacrimal glands drain into nasal
cavities
nasal cavities communicate with
cranial sinuses (air-filled chambers
within the skull)
nasal cavities empty into the
nasopharynx - upper portion of the
pharynx
functions: warm, moisten, and filter
incoming air
Pseudostratified ciliated columnar with goblet
cells lines nasal cavity
-warms air due to high vascularity
-mucous moistens air & traps dust
-cilia move mucous towards pharynx
Nasopharynx
From choanae to soft palate
openings of auditory (Eustachian) tubes from
middle ear cavity
adenoids or pharyngeal tonsil in roof
Passageway for air only
pseudostratified ciliated columnar epithelium
with goblet
From soft palate to epiglottis
fauces is opening from mouth into
oropharynx
palatine tonsils found in side walls, lingual
tonsil in tongue
Common passageway for food & air
stratified squamous epithelium
Oropharynx
Laryngopharynx
Extends from epiglottis to cricoid
cartilage
Common passageway for food &
air & ends as esophagus inferiorly
stratified squamous epithelium
The Pharynx
Tortora & Grabowski 9/e
2000 JWS 23-15
The Larynx
triangular box = voicebox
top of the larynx - hole = glottis with the
epiglottis
Constructed of 3 single & 3 paired
cartilages
Epiglottis---leaf-shaped piece of elastic
cartilage
during swallowing, larynx moves upward
epiglottis bends to cover glottis
thyroid cartilage (Adams apple)
cricoid cartilage
arytenoid cartilage for the attachment of true
vocal cords
functions:
filters, moistens,
vocal
production
Vocal Cords
False vocal cords
(ventricular folds) found
above the true vocal
cords
True vocal cords attach
to arytenoid cartilages
True vocal cord contains
both skeletal muscle and
an elastic ligament (vocal
ligament)
When intrinsic muscles of
the larynx contract they
move the cartilages &
stretch vocal cord tight
When air is pushed past
tight ligament, sound is
produced
The tighter the ligament, the higher the pitch
To increase volume of sound, push air harder
Vocal Cords
Tortora & Grabowski 9/e
2000 JWS 23-18
Trachea
flexible cylindrical tube - Size is 5 in long & 1in diameter
sits anterior (in front of) the esophagus - Extends from larynx to T5
anterior to the esophagus and then splits into bronchi
held upon by C rings of hyaline cartilage = tracheal cartilage
16 to 20 incomplete rings
open side facing esophagus contains smooth muscle
layers:
mucosa = pseudostratified columnar with cilia & goblet cells
submucosa = loose connective tissue & seromucous glands
splits into the right and left primary bronchi - enter the lungs
functions
: conducts
air into the
lungs,
filtration,
moistens
mucosa
submucosa
Trachea and Bronchial Tree
Primary bronchi supply each lung
Secondary bronchi supply each lobe of the lungs (3 right + 2 left)
Tertiary bronchi splits into successive sets of intralobular bronchioles that
supply each bronchopulmonary segment ( right = 10, left = 8)
IL bronchioles split into Terminal bronchioles -> these split into Respiratory
Bronchioles
each RB splits into multiple alveolar ducts which end in an alveolar sac
Structure of Respiratory System
Respiratory zone region of gas exchange occurs only in
respiratory bronchioles and the terminal alveoli sacs
Conducting zone airways that conduct air to the
respiratory zone
Anatomy of the Respiratory Zone
Gas exchange occurs
between the air and
the blood within the
alveoli
Anatomy of the Respiratory Zone
Alveoli (singular is alveolus)
Tiny air sacs clustered at the distal ends of
the alveolar ducts
Alveoli have a thin respiratory membrane
separating the air from blood in pulmonary
capillaries
Respiratory Membrane
The thin alveolar wall consists of:
The fused alveolar and capillary walls
Alveolar epithelial cells
Capillary endothelial cells
The basement membrane
Sandwiched between the alveolar epithelial cells
and the endothelial cells of the capillary
Lung Alveoli and Pulmonary
Capillaries
Gas exchange occurs
across the 300 million
alveoli (60-80 m
2
total
surface area)
Alveolus one cell-layer
thick
Total air-blood barrier
only 2 thin cells across
Between lung air and
blood: 1 alveolar cell
and 1 endothelial cell
Respiratory Membrane
Gas exchanges occurs across the
respiratory membrane
It is < 0.1 m thick
Lends to very efficient diffusion
It is the site of external respiration and
diffusion of gases between the inhaled air
and the blood
Occurs in the pulmonary capillaries
Structures of the Thoracic Cavity
A container with a single opening, the
trachea
Volume of the container changes
Diaphragm moves up and down
Muscles move the rib cage in and out
Volume of the thoracic cavity increases by
enlarging all diameters
diameter = volume
Conducting Zone
Warms and humidifies inspired air reaches respiratory
zone at 37 C
Mucus lining filters and cleans inspired air mucous
moved by cilia to be expectorated
Boyles Law
Volume and pressure are inversely related
volume = pressure
Air always flows from an area of higher
pressure to an area of lower pressure
Decreased pressure in the thoracic cavity in
relation to atmospheric pressure causes air
to flow into the lungs
The process of inspiration
Structures of the Thoracic Cavity
Pleura
Parietal pleura: A membrane that lines the
interior surface of the chest wall
Visceral pleura: A membrane that lines the
exterior surface of the lungs
Intrapleural space
A thin compartment between the two pleurae
filled with intrapleural fluid
Pulmonary Pressures
Pressure gradient
The difference between intrapulmonary and
atmospheric pressures
4 Pulmonary Pressures
Atmospheric pressure
Intra-alveolar (Intrapulmonary) pressure
Intrapleural pressure
Transpulmonary pressure
Pulmonary Pressures
Atmospheric pressure
The pressure exerted by the weight of the air in the
atmosphere (~ 760 mmHg at sea level)
Intra-alveolar (Intrapulmonary) pressure
The pressure inside the lungs
Intrapleural pressure
The pressure inside the pleural space
Transpulmonary pressure
The difference between the intrapleural and intra-
alveolar pressure
Pleural Pressures
Intrapleural pressure
The pressure inside the pleural space or cavity
This cavity contains intrapleural fluid, necessary
for surface tension
Surface tension
The force that holds moist membranes together
due to an attraction that water molecules have
for one another
Responsible for keeping lungs patent
Intrapulmonary and Intrapleural Pressures
During inspiration, intrapulmonary pressure is about -3 mm
Hg pressure; during expiration is about +3 mm Hg
Positive transmural pressure (intrapulmonary minus
intrapleural pressure) keeps lungs inflated
Surface Tension
The force of attraction between liquid
molecules
Type II alveolar cells secrete surfactant
Creates a thin fluid film in the alveoli
Surfactant (a phospholipoprotein) reduces
the surface tension in the alveoli
It interferes with the attraction between fluid
molecules
Decreasing surface tension reduces the
amount of energy required to expand the
lungs
Laplaces Law
Surface Tension
Law of Laplace
states that pressure in
alveolus is directly
proportional to ST; and
inversely to radius of
alveoli
Thus, pressure in smaller
alveoli would be greater
than in larger alveoli, if
ST were same in both
Greater pressure of
smaller alveolus would
cause it to its empty air
into the larger one
Inspiration
Drawing or pulling air into the lungs
Atmospheric pressure forces air into the lungs
The diaphragm moves downward, decreasing
intra-alveolar pressure
The thoracic rib cage moves upward and outward,
increasing the volume of the thoracic cavity
Surface tension
Holds the pleural membranes together, which assists
with lung expansion
Surfactant reduces surface tension within the alveoli
Inspiration
During inspiration, forces are generated that
attempt to pull the lungs away from the
thoracic wall
Surface tension of the intraplueral fluid hold
the lungs against the thoracic wall,
preventing collapse
Expiration
Pushing air out of the lungs
Results due to the elastic recoil of tissues
and due to the surface tension within the
alveoli
Expiration can be aided by:
Thoracic and abdominal wall muscles that pull
the thoracic cage downward and inward,
decreasing intra-alveolar pressure
This compresses the abdominal organs upward
and inward, decreasing the volume of the
thoracic cavity
Muscles of Breathing - Inspiration
Quiet Breathing
Muscles include:
External intercostals
Diaphragm
Contract to expand the rib cage and stretch the
lungs = volume of the thoracic cavity
intrapulmonary volume
intrapulmonary pressure (relative to atmospheric
pressure)
Decreased pressure inside the lungs pulls air into
the lungs down its pressure gradient until
intrapulmonary pressure equals atmospheric
pressure
Forced or Deep Inspiration
Involves several accessory muscles:
Sternocleidomastoid
Pectoralis minor
Scalenes (neck muscles)
Maximal in thoracic volume
Greater in intrapulmonary pressure
More air moves into the lungs
At the end of inspiration, the intrapulmonary
pressure equals atmospheric pressure
Muscles of Breathing - Inspiration
Quiet Breathing
Passive process
Depends on the elasticity of the lungs
Muscles of inspiration relax
The rib cage descends
The lungs recoil
intrapulmonary volume
intrapulmonary pressure
Alveoli are compressed, thus forcing air out
of the lungs
Muscles of Breathing - Expiration
Forced Expiration
It is an active process
Occurs in activities such as blowing up a balloon,
exercising, or yelling
Abdominal wall muscles are involved in forced
expiration
Function to the pressure in the abdominal cavity forcing
the abdominal organs upward against the diaphragm
volume of the thoracic cavity
pressure in the thoracic cavity
Air is forced out of the lungs
Muscles of Breathing - Expiration
Brain (medulla
and higher
centers) sends
impulse to
inspire.
Diaphragm contracts down,
increasing the vertical dimension
of the thorax.
Intercostals and
interchondral
muscles contract
expanding lateral
and anterior-
posterior
dimensions of the
thorax.
Negative air
pressure is
created in the
lungs
Pressure is
equalized
in the
lungs.
Air is
drawn
into the
lungs.
Gas is
expelled
from the
lungs.
Diaphragm and rib-
cage relax
decreasing the
vertical, lateral and
anterior-posterior
dimensions of the
thorax.
Contraction of the
diaphragm,
intercostals and
interchondral
muscles stop and
elastic recoil brings
them to released
position.
Abdominal and
intercostals
muscles contract
decreasing
thoracic volume.
Positive air
pressure is
created in the
lungs.
INSPIRATION
EXPIRATION
Factors Affecting Pulmonary
Ventilation
Lung compliance
The ease with which the lungs may be
expanded, stretched, or inflated
Depends primarily on the elasticity of the
lung tissue
Elasticity refers to the ability of the lung to recoil
after it has been inflated
Factors Affecting Pulmonary
Ventilation
Lung and thoracic cavity tissue has a
natural tendency to recoil, or become
smaller
Lung recoil is essential for normal expiration
and depends on the fibroelastic qualities of
lung tissue
In normal lungs there is a balance between
compliance and elasticity
Recoil pressure is inversely proportional to
compliance
Increased compliance results in decreased recoil
Example: Emphysema
Results in difficulty resuming the shape of the lung
during exhalation
Decreased compliance results in increased recoil
Example: Cysitc fibrosis
Results in difficulty expanding the lung because of
increased fibrous tissue and mucous
Factors Affecting Pulmonary
Ventilation
Airway Resistance (Poiseuilles Law)
Opposition to air flow in the respiratory passageways
Resistance and air flow are inversely related
airway resistance = air flow (and vice versa)
Airway resistance is most affected by changes in the
diameter of the bronchioles
diameter of the bronchioles = airway resistance
Examples:
Asthma
Bronchiospasm during an allergic reaction
A high resistance to air flow produces a greater energy cost
of breathing
Factors Affecting Pulmonary
Ventilation
To Be Continued
You might also like
- Complimentary JournalDocument58 pagesComplimentary JournalMcKey ZoeNo ratings yet
- Canterburytales-No Fear PrologueDocument10 pagesCanterburytales-No Fear Prologueapi-261452312No ratings yet
- Why We Breathe: Functions of the Respiratory SystemDocument9 pagesWhy We Breathe: Functions of the Respiratory SystemZeba ZiaNo ratings yet
- Respiratory System Gas ExchangeDocument64 pagesRespiratory System Gas ExchangenashqonashNo ratings yet
- Respiratory System PDFDocument16 pagesRespiratory System PDFMary Ann SacramentoNo ratings yet
- L11. Respiratory SystemDocument71 pagesL11. Respiratory SystemLimit FtwNo ratings yet
- Anatomy of The Larynx: Thyrohyoid MembraneDocument35 pagesAnatomy of The Larynx: Thyrohyoid MembraneVarsha Shende KhobragadeNo ratings yet
- Respiratory SystemDocument38 pagesRespiratory SystemdjokerNo ratings yet
- Respiratory System ExplainedDocument42 pagesRespiratory System ExplainedSohailriazNo ratings yet
- Handout On GAS EXCHANGEDocument4 pagesHandout On GAS EXCHANGEEli Joshua EvangelistaNo ratings yet
- Respiratory SystemDocument56 pagesRespiratory SystemSalma NawazNo ratings yet
- Anatomy & PhysiologyDocument42 pagesAnatomy & PhysiologyArah Lyn ApiagNo ratings yet
- Respiratory System: Anatomy & PhysiologyDocument111 pagesRespiratory System: Anatomy & PhysiologyJape GarridoNo ratings yet
- 24 - Respiratory SystemDocument18 pages24 - Respiratory SystemHarshil PatelNo ratings yet
- Respiratory System: An Overview of Functions, Anatomy and Gas ExchangeDocument25 pagesRespiratory System: An Overview of Functions, Anatomy and Gas ExchangeKangwa MasekaNo ratings yet
- 22 Respiratory SystemDocument99 pages22 Respiratory SystemvanderphysNo ratings yet
- Anatomy and PhysiologyDocument5 pagesAnatomy and PhysiologyKenNo ratings yet
- The Respiratory System: ASTIKA NUR ROHMAH, S.Kep., NS., M.BiomedDocument43 pagesThe Respiratory System: ASTIKA NUR ROHMAH, S.Kep., NS., M.BiomedAdek KhazeliaNo ratings yet
- Human Biology: Respiratory SystemDocument33 pagesHuman Biology: Respiratory SystemSaikrishna RaoNo ratings yet
- Problems With OxygenationDocument92 pagesProblems With OxygenationEbiNo ratings yet
- Respiratory SystemDocument53 pagesRespiratory SystemRotan CirebonNo ratings yet
- Respiratory System Part 1Document8 pagesRespiratory System Part 1brooklynNo ratings yet
- Respiratory System Functions and AnatomyDocument40 pagesRespiratory System Functions and AnatomychromaNo ratings yet
- CBS RespsystemDocument34 pagesCBS RespsystemtyhbbhhNo ratings yet
- The Respiratory System: Aam Amarullah, M.PDDocument42 pagesThe Respiratory System: Aam Amarullah, M.PDUniversal DiscoveringNo ratings yet
- Anatomy and Physiology of Respiratory SystemDocument34 pagesAnatomy and Physiology of Respiratory SystemSamson SeiduNo ratings yet
- Anatomy, Physiology and Pathology of The RespiratoryDocument68 pagesAnatomy, Physiology and Pathology of The Respiratorytheresia_s_k100% (1)
- Respiratory System 8Document32 pagesRespiratory System 8Naanmatha PuspanathanNo ratings yet
- Functions of The Respiratory SystemDocument10 pagesFunctions of The Respiratory SystemKrisha AvorqueNo ratings yet
- Alterations in OxygenationDocument104 pagesAlterations in OxygenationMelchor Felipe Salvosa100% (1)
- Bronchial AsthmaDocument21 pagesBronchial AsthmaMoonNo ratings yet
- RespiratoryDocument62 pagesRespiratoryDerón Asbery HolmesNo ratings yet
- Respiratory Physiology IDocument47 pagesRespiratory Physiology IDeea LobonțiuNo ratings yet
- Respiration and Gas ExchangeDocument2 pagesRespiration and Gas ExchangeAnime Player ccNo ratings yet
- Roses Are Red, Violets Are Blue, Without Your Lungs Your Blood Would Be, Too.Document249 pagesRoses Are Red, Violets Are Blue, Without Your Lungs Your Blood Would Be, Too.MabesNo ratings yet
- Respiiiraatatoory SystemDocument78 pagesRespiiiraatatoory Systempriyanshuraj717No ratings yet
- Resp 2023 Arsi-1Document118 pagesResp 2023 Arsi-1abenezer isayasNo ratings yet
- Hand Note - Session-1 2Document12 pagesHand Note - Session-1 2Abod AbodNo ratings yet
- Physiology of the Respiratory System-1Document155 pagesPhysiology of the Respiratory System-1Adil MusaddiqNo ratings yet
- Pain, Surgery and Oxygenation NursingDocument7 pagesPain, Surgery and Oxygenation NursingJhoanna de ChavezNo ratings yet
- Lesson 1 Human Breathing SystemDocument37 pagesLesson 1 Human Breathing SystemDavid Lawrence GarciaNo ratings yet
- Physio 1Document17 pagesPhysio 1NeviNo ratings yet
- ANATOMYDocument53 pagesANATOMYJocel Mae OrtegaNo ratings yet
- Care of Clients with Respiratory AlterationsDocument10 pagesCare of Clients with Respiratory AlterationsKamx MohammedNo ratings yet
- Anatomy and physiology of the respiratory systemDocument26 pagesAnatomy and physiology of the respiratory systemRenz Ivan FuntilonNo ratings yet
- AaDocument324 pagesAaBirhanu AyenewNo ratings yet
- Physiology of Respiration - Mechanism of Respiration, GaseousDocument39 pagesPhysiology of Respiration - Mechanism of Respiration, GaseousRakesh KumarNo ratings yet
- Respiratory SystemDocument56 pagesRespiratory SystemLorenz PasensyosoNo ratings yet
- Anatomic and Physiologic OverviewDocument8 pagesAnatomic and Physiologic OverviewJoseph King MacaranasNo ratings yet
- Respiratory SystemDocument31 pagesRespiratory SystemMark Jhosua Austria GalinatoNo ratings yet
- Lecture 6 Respiratory SystemDocument54 pagesLecture 6 Respiratory SystemLouella ArtatesNo ratings yet
- Kuliah 3 Respirasi + CardiovasculerDocument73 pagesKuliah 3 Respirasi + CardiovasculerNindya Alfa DichaNo ratings yet
- Respiratory SystemDocument77 pagesRespiratory SystemJb MoratallaNo ratings yet
- ANATOMY AND PHYSIOLOGY OF THE RESPIRATORY SYSTEMDocument6 pagesANATOMY AND PHYSIOLOGY OF THE RESPIRATORY SYSTEMCarlos Alfonso Borromeo AmoresNo ratings yet
- Respiratory SystemDocument31 pagesRespiratory SystemMary Hyacinthe PalbanNo ratings yet
- Lecture - 5 PDFDocument5 pagesLecture - 5 PDFDavid JokerNo ratings yet
- Supplementary Material 3.1 Basic Concepts and Assessment (N) - 2Document13 pagesSupplementary Material 3.1 Basic Concepts and Assessment (N) - 2Kent Borro CantomayorNo ratings yet
- Breathing and Exchange of GasesDocument25 pagesBreathing and Exchange of GasesSureshNo ratings yet
- Anatomi Pertemuan 4Document52 pagesAnatomi Pertemuan 4dimasNo ratings yet
- Respiratory System GuideDocument8 pagesRespiratory System GuideKhushi JainNo ratings yet
- How Do Humans Breathe? Science Book Age 8 | Children's Biology BooksFrom EverandHow Do Humans Breathe? Science Book Age 8 | Children's Biology BooksNo ratings yet
- Kulpak RSAL - Kesehatan Penyelaman KPLPDocument49 pagesKulpak RSAL - Kesehatan Penyelaman KPLPNabilaNo ratings yet
- Print Lab PaDocument4 pagesPrint Lab PaNabilaNo ratings yet
- Pedoman Nasional Penanggulangan Tuberkulosis 2007Document168 pagesPedoman Nasional Penanggulangan Tuberkulosis 2007inesia_90210100% (27)
- Present Continuous Tense Practice PassageDocument2 pagesPresent Continuous Tense Practice PassageNabilaNo ratings yet
- Print Lab PaDocument4 pagesPrint Lab PaNabilaNo ratings yet
- FED - Summer Term 2021Document18 pagesFED - Summer Term 2021nani chowdaryNo ratings yet
- Journal Sleep Walking 1Document7 pagesJournal Sleep Walking 1Kita SemuaNo ratings yet
- Ifatsea Atsep Brochure 2019 PDFDocument4 pagesIfatsea Atsep Brochure 2019 PDFCondor GuatonNo ratings yet
- Temptations in MinistryDocument115 pagesTemptations in MinistryJoseph Koech100% (1)
- The Seven Kings of Revelation 17Document9 pagesThe Seven Kings of Revelation 17rojelio100% (1)
- Detailed Lesson Plan in MAPEH III I. ObjectivesDocument19 pagesDetailed Lesson Plan in MAPEH III I. ObjectivesJenna FriasNo ratings yet
- Chapter 4. Quality Service and Standards TrainingDocument40 pagesChapter 4. Quality Service and Standards TrainingJia Mae Sapico ApantiNo ratings yet
- Writing A Formal Letter To The PresidentDocument1 pageWriting A Formal Letter To The PresidentPiaAnaisNo ratings yet
- TelanganaDocument16 pagesTelanganaRamu Palvai0% (1)
- Amway Final ReportDocument74 pagesAmway Final ReportRadhika Malhotra75% (4)
- Design of Self - Supporting Dome RoofsDocument6 pagesDesign of Self - Supporting Dome RoofszatenneNo ratings yet
- C++ NotesDocument129 pagesC++ NotesNikhil Kant Saxena100% (4)
- SomDocument191 pagesSomVivek GosaviNo ratings yet
- Canopen-Lift Shaft Installation: W+W W+WDocument20 pagesCanopen-Lift Shaft Installation: W+W W+WFERNSNo ratings yet
- Ultimate Guide To Construction SubmittalsDocument10 pagesUltimate Guide To Construction SubmittalsDavid ConroyNo ratings yet
- E.sybox - Esybox All Information PDFDocument56 pagesE.sybox - Esybox All Information PDFnle_16948No ratings yet
- 09 Chapter TeyyamDocument48 pages09 Chapter TeyyamABNo ratings yet
- IonosondeDocument3 pagesIonosondeFaizan GoharNo ratings yet
- Template - Time in ManufacturingDocument2 pagesTemplate - Time in ManufacturingVero RoaNo ratings yet
- Department of Education Doña Asuncion Lee Integrated School: Division of Mabalacat CityDocument2 pagesDepartment of Education Doña Asuncion Lee Integrated School: Division of Mabalacat CityRica Tano50% (2)
- Jeremy Hughes ReviewDocument5 pagesJeremy Hughes ReviewgracecavNo ratings yet
- Electronics Foundations - Basic CircuitsDocument20 pagesElectronics Foundations - Basic Circuitsccorp0089No ratings yet
- Alfa Romeo Giulia Range and Quadrifoglio PricelistDocument15 pagesAlfa Romeo Giulia Range and Quadrifoglio PricelistdanielNo ratings yet
- Teaching TrigonometryDocument20 pagesTeaching Trigonometryapi-21940065No ratings yet
- Degree and Order of ODEDocument7 pagesDegree and Order of ODEadiba adibNo ratings yet
- ANAPHYDocument23 pagesANAPHYYu, Denise Kyla BernadetteNo ratings yet
- Journal 082013Document100 pagesJournal 082013Javier Farias Vera100% (1)
- Silicone Bonding BrochureDocument4 pagesSilicone Bonding BrochureAmir ShahzadNo ratings yet