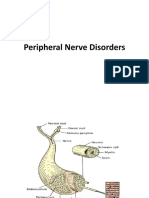
Professional Documents
Culture Documents
Brachial Plexus Injury
Uploaded by
Suci Pramadiani0 ratings0% found this document useful (0 votes)
203 views20 pagesBrachial plexus birth palsy is caused by trauma to the brachial plexus nerves during childbirth, often due to downward or upward traction on the arm. This can lead to muscle imbalance and contractures over time. There are three main types classified by the specific nerves involved. While some cases can be prevented, most cannot be anticipated. The majority of cases recover spontaneously within the first year, while the remaining 20% may require nerve grafting, tendon transfers, or other surgeries to improve function. Prognosis is generally good, with 80% recovering fully, but contractures and sensory loss can occasionally occur without treatment.
Original Description:
Brachial Plexus Injury
Copyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentBrachial plexus birth palsy is caused by trauma to the brachial plexus nerves during childbirth, often due to downward or upward traction on the arm. This can lead to muscle imbalance and contractures over time. There are three main types classified by the specific nerves involved. While some cases can be prevented, most cannot be anticipated. The majority of cases recover spontaneously within the first year, while the remaining 20% may require nerve grafting, tendon transfers, or other surgeries to improve function. Prognosis is generally good, with 80% recovering fully, but contractures and sensory loss can occasionally occur without treatment.
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
203 views20 pagesBrachial Plexus Injury
Uploaded by
Suci PramadianiBrachial plexus birth palsy is caused by trauma to the brachial plexus nerves during childbirth, often due to downward or upward traction on the arm. This can lead to muscle imbalance and contractures over time. There are three main types classified by the specific nerves involved. While some cases can be prevented, most cannot be anticipated. The majority of cases recover spontaneously within the first year, while the remaining 20% may require nerve grafting, tendon transfers, or other surgeries to improve function. Prognosis is generally good, with 80% recovering fully, but contractures and sensory loss can occasionally occur without treatment.
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You are on page 1of 20
Brachial plexus injury->stretch during birth that is
caused by downward or upward traction on the arm
Secondarily, the muscles and bones of the upper
extremity become contracted or deformed over time
because of the resultant muscle imbalance
may not be detected until the baby tries to use the
extremity
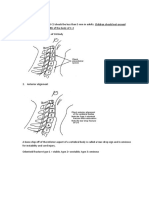
Classification :
Type I (Erb palsy): Injury to roots 4-6 of the cervical
spine
Type II (whole-brachial plexus palsy): C4-T1 involved;
also known as Erb-Duchenne-Klumpkepalsy
Type III (Klumpke palsy): C8-T1 involved
General Prevention
Sometimes obstetricians will advise a caesarean
section if a baby seems extremely large or
cephalopelvic disproportion is present.
Not all cases can be anticipated or prevented
Epidemiology
Incidence
Currently, the incidence is 0.8 per 1,000 live births (2).
This figure is a decline from the rate in 1900, when it was
reported twice as often.
The change most likely results from improved obstetric
care.
Erb palsy is ~4 times as common as Klumpke palsy.
No recognized difference exists in incidence between
boys and girls.
Risk Factors
Fetal malposition
Shoulder dystocia
Cephalopelvic disproportion
High birth weight:
Maternal diabetes
Use of forceps in delivery
Pathophysiology
Pathologic findings vary from stretch to disruption of
the nerves of the brachial plexus (3).
The injury may occur at the cervical foramen as the
nerves exit the spinal canal (poorer prognosis), or
farther down in the neck and shoulder.
Secondary muscle atrophy and contracture ensues.
Etiology
Erb palsy results from downward traction on the
shoulder or arm or lateral traction against the neck.
Klumpke palsy is secondary to upward traction on the
arm.
Both occur because of the force needed in a difficult
extraction.
Associated Conditions
High birth weight
Gestational diabetes
Diagnosis
Signs and Symptoms
Decreased active use of the extremity
Arm held in internal rotation (2)
Loss of full active or passive external rotation
Inability to abduct (raise) the shoulder
Atrophy of the involved muscles (late) (Fig. 1)
Elbow flexion contracture
Possible Horner syndrome in Klumpke palsy
The condition is not painful.
A loss of sensation may be noted with complete plexus
injuries.
History
Decreased infant arm movements sometimes are noted from birth.
In other cases, more subtle decreases in shoulder movement or
presence of arm contracture may not be noted until later.
Physical Exam
Physical examination is the primary means of diagnosis.
Palpate for tenderness over the clavicle, proximal humerus, and ribs.
Test sensation by responses to light touch or pinch.
Test the function of all muscles in the shoulder, elbow, and hand by
stimulation and observation.
In patients with Erb palsy, the shoulder is internally rotated and lacks
external rotation and abduction.
In Klumpke palsy, loss of finger and interosseous function occurs.
12
17
13
17
Tests
Imaging
Plain radiographs often are indicated at birth to rule
out other injuries that may cause decreased movement
of the infant's arm (clavicle fracture, proximal
humerus fracture); such injuries may coexist with
brachial plexus birth palsy.
At the time of late reconstruction in a child >4 years
old who has residual shoulder imbalance, plain
radiographs and CT scans are indicated to assess the
shape of the glenohumeral joint.
Diagnostic Procedures/Surgery
An electromyogram should be obtained if no clinical
return of deltoid or biceps function occurs by 36
months of age.
Lack of reinnervation may be a relative indication for surgery.
Cervical myelography may be helpful for diagnosing the
level of injury.
Meningoceles seen at the root levels in the cervical spinal
cord indicate that roots were avulsed from the cord, and the
prognosis is poor.
A finding of meningoceles indicates that different strategies
may be needed at surgery.
Differential Diagnosis
Clavicle fracture:
Usually painful to palpation
Some shoulder motion may be elicited.
Proximal humeral physeal fracture:
Same findings as clavicle fracture, with tenderness over the
proximal humerus; the abnormality may not show on radiographs
because the proximal humerus is not ossified at birth.
Ultrasound or MRI studies may be diagnostic, as are plain films
710 days later.
Septic arthritis of the shoulder:
May cause pseudoparalysis
Fever in the newborn may not be pronounced.
Treatment
General Measures
Parents should stretch the infant's arm several times a day as
directed by the occupational therapist (13).
The patient should be referred to a specialized pediatric
orthopaedic surgeon for monitoring and decision-making.
Observation and passive ROM are indicated for the newborn;
80% of patients recover spontaneously by 1 year of age (4).
Splinting is not necessary, but continued follow-up is needed.
Surgery is indicated for the remaining 20% of patients, with
grafting of the injured nerves (if no meningoceles are present
and the elapsed time is not >2 years) or with tendon transfers to
improve muscle balance .
Activity
No restrictions
Encourage passive ROM.
Special Therapy
Physical Therapy
An occupational therapist is helpful in teaching the parents
how to stretch and what contractures to watch for.
Splinting is not needed, but stretching and passive ROM
are encouraged.
Surgery
Nerve repair/reconstruction:
May be performed with an operative microscope with direct repair or
grafting of the injured nerves if the patient's function does not return
in ~6 months.
The exact timing is controversial.
Tendon transfers may be performed later to restore external rotation to
the shoulder.
Release of the tight internal rotators also may be indicated.
Humeral osteotomy is another way to restore an externally rotated
position.
Several muscle transfers are available to restore elbow flexion, most
notably the latissimus transfer.
Transfers for finger and wrist function are least commonly needed.
Follow-up
Issues for Referral
It is important to refer the baby with brachial birth palsy to an orthopaedic
surgeon with an interest in this condition because it is a specialized field.
Prognosis
80% of patients with brachial plexus birth palsy recover spontaneously.
Surgery may help many of the remainder.
Complications
Contracture of shoulder, elbow, or wrist
Affected extremity smaller in length and girth
Sensory loss
Shoulder dislocation
Patient Monitoring
The patient should be seen approximately every 23 months to look for
return of function and to plan for appropriate diagnostic testing.
You might also like
- Volkmann's Ischemic ContractureDocument41 pagesVolkmann's Ischemic ContractureAayush AryalNo ratings yet
- Preventable Death: Dco: DR Thit Lwin School of Medicine UMSDocument56 pagesPreventable Death: Dco: DR Thit Lwin School of Medicine UMSStar CruiseNo ratings yet
- Salter 15Document70 pagesSalter 15Kahfi Rakhmadian KiraNo ratings yet
- Damage Control Orthopedic - ASWDocument32 pagesDamage Control Orthopedic - ASWAisyah KhumairahNo ratings yet
- Chronic Limb IschemiaDocument29 pagesChronic Limb IschemiaSadia NaveedNo ratings yet
- Tg13: Updated Tokyo Guidelinesfor Acute CholecystitisDocument59 pagesTg13: Updated Tokyo Guidelinesfor Acute CholecystitisDeoValendraNo ratings yet
- CTEV AmsDocument22 pagesCTEV AmsDavin Silalahi100% (1)
- Acute Abdomen and PeritonitisDocument17 pagesAcute Abdomen and PeritonitisAnisaPratiwiArumningsihNo ratings yet
- Peripheral Nerve DisordersDocument75 pagesPeripheral Nerve DisordersAllahbesertkitaNo ratings yet
- Radiographic Anatomy of VertebraeDocument32 pagesRadiographic Anatomy of VertebraeRienaAbrahamsNo ratings yet
- Amputation FingerDocument36 pagesAmputation Fingerlolianton87No ratings yet
- Ganglion of The Hand and WristDocument13 pagesGanglion of The Hand and WristtantraNo ratings yet
- Chronic Limb Threatening IschemiaDocument35 pagesChronic Limb Threatening Ischemiasifatullah khanNo ratings yet
- Cervical Spine X RayDocument5 pagesCervical Spine X Rayanz_4191No ratings yet
- Acetabular and Hip FractureDocument133 pagesAcetabular and Hip FractureJuanita HenryNo ratings yet
- Tendon InjuriesDocument48 pagesTendon InjuriesdiasNo ratings yet
- Introduction of MSK ImagingDocument63 pagesIntroduction of MSK ImagingyeabsraNo ratings yet
- PCL's Avulsion FractureDocument22 pagesPCL's Avulsion FractureNey da OnneyNo ratings yet
- ClubfootDocument52 pagesClubfootArianto PrabowoNo ratings yet
- Excision of Branchial Cleft CystsDocument10 pagesExcision of Branchial Cleft Cystssjs315No ratings yet
- Ankle Anatomy and Blood Supply of TalusDocument66 pagesAnkle Anatomy and Blood Supply of TalusShashank29 LakkalaNo ratings yet
- Principles of Management of Soft Tissue SarcomaDocument33 pagesPrinciples of Management of Soft Tissue Sarcomabashiruaminu100% (1)
- Atelektasis: Penyaji: Martvera SDocument20 pagesAtelektasis: Penyaji: Martvera Saidil ilham100% (1)
- Fracture ComplicationDocument29 pagesFracture Complicationlgtoalejandro100% (1)
- Fingertip and Nail Bed InjuriesDocument27 pagesFingertip and Nail Bed InjuriesiwanbaongNo ratings yet
- Skull Cervical X-RayDocument15 pagesSkull Cervical X-RayAwal AlfitriNo ratings yet
- To TiroidDocument67 pagesTo TiroidfaisaldanyaniNo ratings yet
- FlapDocument4 pagesFlapMd Ahsanuzzaman PinkuNo ratings yet
- Anterolateral Thigh - ALT - Free Flap For Head and Neck ReconstructionDocument12 pagesAnterolateral Thigh - ALT - Free Flap For Head and Neck ReconstructionАрман ЖуманкуловNo ratings yet
- Management of Avn HipDocument13 pagesManagement of Avn Hipterencedsza100% (1)
- Critical Limb IschemiaDocument29 pagesCritical Limb IschemiadockunNo ratings yet
- Trauma Spinal Wates Dr. WRDocument68 pagesTrauma Spinal Wates Dr. WRLanlan LesmanaNo ratings yet
- Upper Extremity FracturesDocument80 pagesUpper Extremity FracturesSidan EmozieNo ratings yet
- Acute Pancreatitis: Methas Arunnart MD. Songkhla HospitalDocument70 pagesAcute Pancreatitis: Methas Arunnart MD. Songkhla HospitalMohd ImranNo ratings yet
- Tracheostomy: Indications and ProcedureDocument10 pagesTracheostomy: Indications and ProcedureAinur AbdrakhmanovaNo ratings yet
- I. X-Ray Image: Hindfoot Fractures By: Jeremy Tan and Sarah HillDocument8 pagesI. X-Ray Image: Hindfoot Fractures By: Jeremy Tan and Sarah HillSheril MarekNo ratings yet
- Ankle ComplexDocument95 pagesAnkle ComplexMangala Prema MohanarangamNo ratings yet
- Articular Fractures: PrinciplesDocument24 pagesArticular Fractures: Principlestom kurniawanNo ratings yet
- Trochanteric #Document20 pagesTrochanteric #Prakash AyyaduraiNo ratings yet
- 3 - Flail ChestDocument3 pages3 - Flail ChestKrishna Chaitanya GovardhanamNo ratings yet
- Craniotomy FlapsDocument41 pagesCraniotomy FlapsKaramsi Gopinath NaikNo ratings yet
- Anatomy and Physiology of Small and Large Intestines, Rectum and AnusDocument24 pagesAnatomy and Physiology of Small and Large Intestines, Rectum and AnusElmer PatrickNo ratings yet
- Perioperative Management 1203114432600412 4Document53 pagesPerioperative Management 1203114432600412 4polushkyNo ratings yet
- Thyroid Cancer Diagnosis and ManagementDocument45 pagesThyroid Cancer Diagnosis and Managementapi-3704562100% (1)
- Radiography of The Hip: Lines, Signs, and Patterns of DiseaseDocument16 pagesRadiography of The Hip: Lines, Signs, and Patterns of DiseaseVivi Evita DewiNo ratings yet
- Surgery of PancreasDocument30 pagesSurgery of PancreasmackieccNo ratings yet
- Anorectal Anatomy & Surgical ManagementDocument164 pagesAnorectal Anatomy & Surgical Managementsgod34No ratings yet
- Summary Anatomy of Large IntestineDocument2 pagesSummary Anatomy of Large IntestinesahirbuleNo ratings yet
- EktremitasDocument40 pagesEktremitasBram wijayaNo ratings yet
- Gastric Perforation in The Newborn: Ai-Xuan Le Holterman, M.DDocument23 pagesGastric Perforation in The Newborn: Ai-Xuan Le Holterman, M.Dpldhy2004No ratings yet
- Arm:Leg Fracture PDFDocument11 pagesArm:Leg Fracture PDFHannaNo ratings yet
- Ctev NewDocument48 pagesCtev NewDhinie NovianiNo ratings yet
- 2013 - Pancreaticoduodenectomy (Whipple Procedure) TechniquesDocument11 pages2013 - Pancreaticoduodenectomy (Whipple Procedure) TechniquesOlteanu IonutNo ratings yet
- Avascular Necrosis of The Fibular SesamoidDocument7 pagesAvascular Necrosis of The Fibular SesamoidAlex Yvan Escobedo HinostrozaNo ratings yet
- BREAST Development TSADocument62 pagesBREAST Development TSAshirley_ling_15100% (1)
- Below Knee and Through Knee ProsthesisDocument4 pagesBelow Knee and Through Knee ProsthesisClang TejadaNo ratings yet
- TractionDocument39 pagesTractionLu IsNo ratings yet
- Amputasi Bellow KneeDocument29 pagesAmputasi Bellow KneeMolgen PanjaitanNo ratings yet
- Stenosing Tenosynovitis, (Trigger Finger) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandStenosing Tenosynovitis, (Trigger Finger) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- PALSYDocument10 pagesPALSYGuhan SubramaniamNo ratings yet
- OsteomyelitisDocument32 pagesOsteomyelitisAndi Wija Indrawan PangerangNo ratings yet
- Hyperbaric Oxygen As An Adjuvant Treatment For Malignant Otitis ExternaDocument11 pagesHyperbaric Oxygen As An Adjuvant Treatment For Malignant Otitis ExternaSuci PramadianiNo ratings yet
- Malignant Otitis External-Our Experience: R. B. Sardesai, T. KrishnakumarDocument4 pagesMalignant Otitis External-Our Experience: R. B. Sardesai, T. KrishnakumarSuci PramadianiNo ratings yet
- Malignant Otitis Externa in Patients With Diabetes Mellitus: Case ReportDocument0 pagesMalignant Otitis Externa in Patients With Diabetes Mellitus: Case ReportSuci PramadianiNo ratings yet
- Malignant Otitis Externa 20070821Document0 pagesMalignant Otitis Externa 20070821Suci PramadianiNo ratings yet
- 2018 Annual Report MedShareDocument28 pages2018 Annual Report MedShareBrain ZonaNo ratings yet
- Leave of Absence: Republic Act (RA) No. 11210Document9 pagesLeave of Absence: Republic Act (RA) No. 11210Bigz MaxNo ratings yet
- The Reproductive System The Reproductive System: © 2018 Pearson Education, Ltd. 1Document19 pagesThe Reproductive System The Reproductive System: © 2018 Pearson Education, Ltd. 1lourd nabNo ratings yet
- Genital Tract InjuriesDocument16 pagesGenital Tract InjuriesNadiya Rashid100% (4)
- Luma - Health Insurance Quotation - May Kabyar Oo (3 Options)Document3 pagesLuma - Health Insurance Quotation - May Kabyar Oo (3 Options)Kabyar MayNo ratings yet
- Stages of LaborDocument5 pagesStages of Laborchrisanne09No ratings yet
- Management of Normal LaborDocument98 pagesManagement of Normal LaborGoogle SecurityNo ratings yet
- Vital StatisticsDocument35 pagesVital StatisticsRadha100% (1)
- Assess Knowledge and Practice Regarding Partograph Among Staff Nurses: Pre Experimental StudyDocument5 pagesAssess Knowledge and Practice Regarding Partograph Among Staff Nurses: Pre Experimental StudyDiksha chaudharyNo ratings yet
- Preterm Labor: Dr. Cecille Rapal-GamboaDocument20 pagesPreterm Labor: Dr. Cecille Rapal-GamboaKatNo ratings yet
- Municipal Health Office Municipality of Claveria, CagayanDocument2 pagesMunicipal Health Office Municipality of Claveria, CagayanSophia Kaye AguinaldoNo ratings yet
- Operational Guidelines-Use of Antenatal Corticosteroids in Preterm LabourDocument32 pagesOperational Guidelines-Use of Antenatal Corticosteroids in Preterm LabourPriyaancaHaarshNo ratings yet
- Pregnancy ExaminationDocument11 pagesPregnancy ExaminationLisa KnappNo ratings yet
- Case Study - Full-Term BabyDocument32 pagesCase Study - Full-Term BabyMarron Jane GanoticeNo ratings yet
- Which Is The Primary Goal of Community Health NursingDocument20 pagesWhich Is The Primary Goal of Community Health NursingKeepItSecretNo ratings yet
- A Conceptual Guide To MRCP (Uk) Paces Exam.: Station 2, 4 and 5. SampleDocument29 pagesA Conceptual Guide To MRCP (Uk) Paces Exam.: Station 2, 4 and 5. Samplesoe100% (1)
- Dystocia: Presented By:kushal Neupane Roll No:13 B.V.SC & A.H 8 Semester HicastDocument19 pagesDystocia: Presented By:kushal Neupane Roll No:13 B.V.SC & A.H 8 Semester Hicastkushal NeupaneNo ratings yet
- Psychiatric Disorders in PregnancyDocument93 pagesPsychiatric Disorders in Pregnancyjinijinu100% (3)
- Community Health Program in Sundarbans: About The ApplicantDocument26 pagesCommunity Health Program in Sundarbans: About The ApplicantAnup PaudelNo ratings yet
- Malposition - Malpresentation (L)Document35 pagesMalposition - Malpresentation (L)Touseef Ur RehmanNo ratings yet
- Situation Analysis of Community Midwives ' Training in SindhDocument107 pagesSituation Analysis of Community Midwives ' Training in Sindhmidwifepak100% (1)
- EmdrDocument33 pagesEmdrShanker Iyer100% (1)
- Case PresDocument26 pagesCase PresRenz BaldonNo ratings yet
- Radu Cinamar - Peter Moon - Transylvanian Sunrise (2003)Document282 pagesRadu Cinamar - Peter Moon - Transylvanian Sunrise (2003)lennardvandergraafNo ratings yet
- BSM M104 Curriculum OutlineDocument3 pagesBSM M104 Curriculum OutlineDamaris Pandora Songcal0% (1)
- Physiologic Assessment of Newborn, Newborn Adaptation and Normal Growth & DevelopmentDocument4 pagesPhysiologic Assessment of Newborn, Newborn Adaptation and Normal Growth & DevelopmentBernard M. Lapuz FullNo ratings yet
- Neuropsycholgical Assessment IgnouDocument29 pagesNeuropsycholgical Assessment IgnouFiroz AhmedNo ratings yet
- O&G Clerking ScriptDocument4 pagesO&G Clerking ScriptA VHRSENo ratings yet
- Written Report in NCM107Document5 pagesWritten Report in NCM107Marifel Sombreno PeñarandaNo ratings yet
- AMC Clinical Psychiatry NoteDocument59 pagesAMC Clinical Psychiatry NoteShahriar Ahmed Sujoy100% (3)