Professional Documents
Culture Documents
Idaho Duals Demonstration Stakeholder PP
Uploaded by
Mark Reinhardt0 ratings0% found this document useful (0 votes)
32 views11 pagessource: healthandwelfare.idaho.gov
Original Title
Idaho Duals Demonstration Stakeholder Pp
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentsource: healthandwelfare.idaho.gov
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
32 views11 pagesIdaho Duals Demonstration Stakeholder PP
Uploaded by
Mark Reinhardtsource: healthandwelfare.idaho.gov
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 11
Centers for Medicare & Medicaid
Services & Idaho Department of
Health and Welfare Demonstration
to Integrate Care for Dual Eligible
Individuals
Idaho Medicare-Medicaid
Coordinated Plan (MMCP)
Stakeholder Update
June 5, 2013
Webinar Topics
Plan Benefit Package
RFP versus Contract
Timeline
Implementation- phased in approach
MOU
Readiness Review
2
Plan Benefit Package (PBP)
The PBP is a list of Medicare and Medicaid
benefits Health Plans will offer in the
Demonstration
All Medicare and Medicaid benefits, unless
otherwise carved out as in the case of
Developmental Disabilities services, are required
CMS required Health Plans to submit a PBP by
June 3, 2013
3
Plan Benefit Package (PBP)
Two Health Plans have submitted PBPs for the
Demonstration
CMS provided a template to IDHW to provide
PBP guidance to Health Plans for services that
may have Medicaid benefit limitations greater
than Medicare benefit limitations
4
Plan Benefit Package (PBP)
IDHW posted guidance on Medicaid benefits and
answers to PBP-related questions at:
www.MedicaidLTCManagedCare.dhw.idaho.gov
PBP includes benefit limitations, cost sharing
information, prior authorization requirements, and
other notes. Health Plans must be at least as Enrollee-
friendly as Medicaid.
Benefit limitations example: 12 hours/day limitation for
adult day health.
Cost sharing information example: possible $3.65
copayments for specified services
Prior authorization requirements, if applicable
Other notes to clarify the nature of a benefit
5
RFP vs. Contract
IDHW requested an exemption to the
competitive bid process - request approved by
the Department of Purchasing
This means we move directly to contract
negotiations
Process will involve release of the contract to the
interested health plans for review and bid, along
with a questionnaire
Plans will submit their bid and their responses
to the questionnaire for evaluation by IDHW
6
Timeline for Phased-In Enrollment
Approach
Enrollment in the Demonstration will be phased in by IDHWs three
geographical service areas (Southwest, East and North).
Opt-in enrollment in the Southwest geographic area begins on March 1,
2014.
All Enrollees in the Southwest geographic area who have not opted-in or
out before April 1, 2014 will be passively enrolled on that date.
Opt-in enrollment in the East geographic area begins on May 1, 2014.
All Enrollees in the East geographic area who have not opted-in or out
before June 1, 2014 will be passively enrolled on that date.
Opt-in enrollment in the North geographic area begins on July, 1, 2014.
All Enrollees in the North geographic area who have not opted-in or out
before August, 1, 2014 will be passively enrolled on that date.
7
Tasks and Timeline for April 1, 2014
Implementation
8
Key Timeline Step Target Dates
Plans submitted integrated Plan Benefit Packages to CMS June 3, 2013
Plans submit supplemental formulary files, including the
Additional Demonstration Drug (ADD) file, in HPMS
June 7, 2013
MOU Signed July, 2013
State releases contract and questionnaire for Medicaid
only services to interested organizations for review & bid
July, 2013
Plans selected by State August, 2013
Readiness Reviews Aug. Nov. 2013
State submits 1915(c) amendments October, 2013
State submits 1915(b) waiver application October, 2013
Contract shared with plans and the State
November 15,
2013
Tasks and Timeline for April 1, 2014
Implementation cont.
9
Key Timeline Step Target Dates
Health Home SPA submitted if needed December 1, 2013
Coordinated Benchmark SPA December 1, 2013
State and Health Plan Sign contract December, 2013
60-day beneficiary notice sent in Area One (State) January, 2014
Plan Marketing begins February 1, 2014
Opt-in service coverage begins in Area One March 1, 2014
30-day beneficiary notice sent in Area One (State) March 1, 2014
Passive Enrollment takes effect in Area One April 1, 2014
Passive Enrollment takes effect in Area Two June 1, 2014
Passive Enrollment takes effect in Area Three August 1, 2014
Questions?
LTCmanagedcare@dhw.idaho.gov
Website
http://www.MedicaidLTCManagedCare.d
hw.idaho.gov
Duals Demonstration Feedback
11
You might also like
- Michigan Medicaid Presumptive EligibilityDocument3 pagesMichigan Medicaid Presumptive EligibilityBeverly TranNo ratings yet
- EHR and Meaningful UseDocument4 pagesEHR and Meaningful UseNkeletseng MakakaNo ratings yet
- Ohio MCPDocument4 pagesOhio MCPseppun1No ratings yet
- Motion Picture Health Plan Appeals - NoticeDocument6 pagesMotion Picture Health Plan Appeals - Noticeravip3366No ratings yet
- 2023 Medicare KickoffDocument27 pages2023 Medicare KickofflollieNo ratings yet
- AchievingMeaningfulUse Stage2 PDFDocument13 pagesAchievingMeaningfulUse Stage2 PDFAnonymous c0zdLnNo ratings yet
- 01-005.16 Food CodeDocument1 page01-005.16 Food Codesuperm0mof6No ratings yet
- ANDA Submissions - Prior Approval Supplements Under GDUFADocument14 pagesANDA Submissions - Prior Approval Supplements Under GDUFASreekanth ChNo ratings yet
- Ryan White HIV-AIDS Program Moving ForwardDocument53 pagesRyan White HIV-AIDS Program Moving ForwardAntonio CardozoNo ratings yet
- HCRprovisions - Older Adults 3-30-10Document6 pagesHCRprovisions - Older Adults 3-30-10hcreformNo ratings yet
- The Impact of The Economic Recovery Act of 2009 On HealthcareDocument31 pagesThe Impact of The Economic Recovery Act of 2009 On Healthcareasg_akn8335No ratings yet
- Egwp 11 06 13 User Call PresentationDocument61 pagesEgwp 11 06 13 User Call PresentationHerb ZydneyNo ratings yet
- Ms. Usha Tyagi, 35, Anand Lok, Rurkee Road, Meerut-Uttar Pradesh, IndiaDocument5 pagesMs. Usha Tyagi, 35, Anand Lok, Rurkee Road, Meerut-Uttar Pradesh, IndiaAdrishyaNo ratings yet
- HLFL Clean Air Global Application CriteriaDocument3 pagesHLFL Clean Air Global Application CriteriaЭма СэмNo ratings yet
- Healthcare Trans From at Ion WaiverDocument34 pagesHealthcare Trans From at Ion WaiverGovtfraudlawyerNo ratings yet
- Groom Webinar - Tri-Agencies Meet Deadline With First Set of Surprise Billing Rules With More To Come (July 29 2021)Document40 pagesGroom Webinar - Tri-Agencies Meet Deadline With First Set of Surprise Billing Rules With More To Come (July 29 2021)Tammy KillionNo ratings yet
- PMD Oral Health Care PlanDocument2 pagesPMD Oral Health Care PlanAlpha SniperNo ratings yet
- Nebraska Wellness Options - 2011 CSG Innovations Award WinnerDocument7 pagesNebraska Wellness Options - 2011 CSG Innovations Award Winnerbvoit1895No ratings yet
- FEHB Program Carrier Letter: All CarriersDocument8 pagesFEHB Program Carrier Letter: All CarriersleejolieNo ratings yet
- 2015 5-Star Plan Ratings Overview Job AidDocument2 pages2015 5-Star Plan Ratings Overview Job AidTrisha LaragaNo ratings yet
- Ms. Dr. Aparajita C/o D. S. Verma, A-137, Defence Colony, Mawana Road, Meerut-UP IndiaDocument5 pagesMs. Dr. Aparajita C/o D. S. Verma, A-137, Defence Colony, Mawana Road, Meerut-UP IndiaAdrishyaNo ratings yet
- Benzie County Draft Opioid Settlement RFPDocument8 pagesBenzie County Draft Opioid Settlement RFPColin MerryNo ratings yet
- BSA Benefits ProgramDocument45 pagesBSA Benefits Programb_v_k_1979No ratings yet
- WHO - HMN Guideline For Application To Strengthen National HIS Under GAVI HSS Funding 2009Document4 pagesWHO - HMN Guideline For Application To Strengthen National HIS Under GAVI HSS Funding 2009HarumNo ratings yet
- Nysarsc Presentation June 2014Document40 pagesNysarsc Presentation June 2014api-247460702No ratings yet
- Dr. SchumacherLooking in The Crystal Ball - 2012 and HospiceDocument42 pagesDr. SchumacherLooking in The Crystal Ball - 2012 and HospicemollayoNo ratings yet
- 01.08.13 BOC Agenda Packet For Ipad FinalDocument40 pages01.08.13 BOC Agenda Packet For Ipad FinalThunder PigNo ratings yet
- Norton BenefitsDocument48 pagesNorton BenefitsTNo ratings yet
- Power Point Conversion ProviderMeeting 8.1.13Document31 pagesPower Point Conversion ProviderMeeting 8.1.13janbullingtonNo ratings yet
- Critical Review of NHSS-IP - Sagar ParajuliDocument45 pagesCritical Review of NHSS-IP - Sagar ParajuliSagar ParajuliNo ratings yet
- Part D PowerpointDocument14 pagesPart D PowerpointMark ReinhardtNo ratings yet
- Managed Care Waivers - Spas 09 2015 RevisedDocument3 pagesManaged Care Waivers - Spas 09 2015 Revisedapi-293754603No ratings yet
- Flexi Medical Plan BrochureDocument28 pagesFlexi Medical Plan BrochurewoodksdNo ratings yet
- Medicare Module 1 Program Basics Download PDFDocument62 pagesMedicare Module 1 Program Basics Download PDFjohndeleon0No ratings yet
- Managed Care NPRM 09 2015Document3 pagesManaged Care NPRM 09 2015api-293754603No ratings yet
- English 1103 Research PresentationDocument18 pagesEnglish 1103 Research PresentationZnaLeGrandNo ratings yet
- Infosys Infosys 2014Document45 pagesInfosys Infosys 2014Basant KumarNo ratings yet
- LRP Application GuidanceDocument74 pagesLRP Application GuidanceStarrx714No ratings yet
- CPRNYDE Response To The 2012 DOH Report - April 5 2013Document31 pagesCPRNYDE Response To The 2012 DOH Report - April 5 2013EdmondsonNo ratings yet
- Winterbourne Progress Meeting Sir Stephen Bubb: 7 December 2015 Coin Street Neighbourhood CentreDocument69 pagesWinterbourne Progress Meeting Sir Stephen Bubb: 7 December 2015 Coin Street Neighbourhood CentreInclusionNorthNo ratings yet
- GP&SP Presentation Slide-BiDocument23 pagesGP&SP Presentation Slide-BirxzlajuNo ratings yet
- State Health Exchanges and Qualified Health PlansDocument49 pagesState Health Exchanges and Qualified Health PlansRajiv GargNo ratings yet
- 2015 Anthem Small Group 4-1-2015 Rate Filing PDFDocument40 pages2015 Anthem Small Group 4-1-2015 Rate Filing PDFmoconsumerNo ratings yet
- RFP Compensation Package Survey (14th Feb)Document5 pagesRFP Compensation Package Survey (14th Feb)AdrishyaNo ratings yet
- Final AmendementDocument82 pagesFinal AmendementDegrace NsNo ratings yet
- Capitation: Senior Health Financing ExpertDocument12 pagesCapitation: Senior Health Financing ExpertNgô Xuân ThủyNo ratings yet
- Ehr Selection: Fall 2009 Idn Summit Peer-To-Peer Learning Exchange Research ReportsDocument9 pagesEhr Selection: Fall 2009 Idn Summit Peer-To-Peer Learning Exchange Research Reportsraduben5403No ratings yet
- Arpa Planning Proposal FinalDocument10 pagesArpa Planning Proposal FinalTitus WuNo ratings yet
- Updates On The Implementation of Health Reforms and The Millennium Development GoalsDocument31 pagesUpdates On The Implementation of Health Reforms and The Millennium Development GoalsSeriel TismoNo ratings yet
- Healthcare Reform Resource Guide and Fact Book - March2009Document37 pagesHealthcare Reform Resource Guide and Fact Book - March2009SEIUOnlineNo ratings yet
- Health - Exam Material 2021 RevisedDocument51 pagesHealth - Exam Material 2021 Revisedraj kishan srinivasanNo ratings yet
- Transition To Compliant Policies 03-06-2015Document7 pagesTransition To Compliant Policies 03-06-2015Becket AdamsNo ratings yet
- AHM 250 SummaryDocument116 pagesAHM 250 SummaryDinesh Anbumani100% (5)
- Primary Care Rural Innovative Multidisciplinary Models GO4600 - Frequently Asked QuestionsDocument4 pagesPrimary Care Rural Innovative Multidisciplinary Models GO4600 - Frequently Asked QuestionsJennifer DoggettNo ratings yet
- Nurse Deployment ProjectDocument6 pagesNurse Deployment ProjectAngel022150% (2)
- 2015 Humana Small Group Rate Filing PDFDocument19 pages2015 Humana Small Group Rate Filing PDFmoconsumerNo ratings yet
- September 16, 2014, Tentative Agreement Questions and Answers For Members Information and Procedures For VotingDocument2 pagesSeptember 16, 2014, Tentative Agreement Questions and Answers For Members Information and Procedures For VotingMartinvandenHemelNo ratings yet
- Health Care Reform Act: Critical Tax and Insurance RamificationsFrom EverandHealth Care Reform Act: Critical Tax and Insurance RamificationsNo ratings yet
- Textbook of Urgent Care Management: Chapter 37, Setting Up a Health-Care Compliance ProgamFrom EverandTextbook of Urgent Care Management: Chapter 37, Setting Up a Health-Care Compliance ProgamNo ratings yet
- Patrol LP Scenario03 July2021Document25 pagesPatrol LP Scenario03 July2021Mark ReinhardtNo ratings yet
- WW Idaho Power Co. - Natural Gas Plant Cooling Water Draft PermitDocument27 pagesWW Idaho Power Co. - Natural Gas Plant Cooling Water Draft PermitMark ReinhardtNo ratings yet
- H0001Document2 pagesH0001Mark ReinhardtNo ratings yet
- Sustainability of Idaho's Direct Care Workforce (Idaho Office of Performance Evaluations)Document80 pagesSustainability of Idaho's Direct Care Workforce (Idaho Office of Performance Evaluations)Mark ReinhardtNo ratings yet
- 20221230final Order No 35651Document5 pages20221230final Order No 35651Mark ReinhardtNo ratings yet
- MMCP CY2023 Idaho Blue Cross Medicaid ContractDocument185 pagesMMCP CY2023 Idaho Blue Cross Medicaid ContractMark ReinhardtNo ratings yet
- Patrol LP Scenario04 July2021Document24 pagesPatrol LP Scenario04 July2021Mark ReinhardtNo ratings yet
- 20200206press Release IPC E 18 15Document1 page20200206press Release IPC E 18 15Mark ReinhardtNo ratings yet
- The First Rules of Los Angeles Police DepartmentDocument1 pageThe First Rules of Los Angeles Police DepartmentMark ReinhardtNo ratings yet
- A Bill: 117 Congress 1 SDocument22 pagesA Bill: 117 Congress 1 SMark ReinhardtNo ratings yet
- Transitioning Coal Plants To Nuclear PowerDocument43 pagesTransitioning Coal Plants To Nuclear PowerMark ReinhardtNo ratings yet
- Affidavit Writing Made EasyDocument6 pagesAffidavit Writing Made EasyMark ReinhardtNo ratings yet
- Crime Scene Manual Rev3Document153 pagesCrime Scene Manual Rev3Mark ReinhardtNo ratings yet
- Bills 113s987rsDocument44 pagesBills 113s987rsMark ReinhardtNo ratings yet
- NIYSTXDocument19 pagesNIYSTXMark ReinhardtNo ratings yet
- A Bill: 116 Congress 2 SDocument15 pagesA Bill: 116 Congress 2 SMark ReinhardtNo ratings yet
- HJR003Document1 pageHJR003Mark ReinhardtNo ratings yet
- City of Boise Housing Bonus Ordinance and Zoning Code Rewrite MemoDocument11 pagesCity of Boise Housing Bonus Ordinance and Zoning Code Rewrite MemoMark ReinhardtNo ratings yet
- NIYSWADocument17 pagesNIYSWAMark ReinhardtNo ratings yet
- Idaho H0098 2021 SessionDocument4 pagesIdaho H0098 2021 SessionMark ReinhardtNo ratings yet
- NIYSVADocument15 pagesNIYSVAMark ReinhardtNo ratings yet
- NIYSTNDocument5 pagesNIYSTNMark ReinhardtNo ratings yet
- NIYSUTDocument4 pagesNIYSUTMark ReinhardtNo ratings yet
- NIYSVTDocument4 pagesNIYSVTMark ReinhardtNo ratings yet
- NIYSSCDocument11 pagesNIYSSCMark ReinhardtNo ratings yet
- NIYSPRDocument7 pagesNIYSPRMark ReinhardtNo ratings yet
- NIYSSDDocument4 pagesNIYSSDMark ReinhardtNo ratings yet
- NIYSWIDocument8 pagesNIYSWIMark ReinhardtNo ratings yet
- NIYSRIDocument9 pagesNIYSRIMark ReinhardtNo ratings yet
- NIYSPADocument8 pagesNIYSPAMark ReinhardtNo ratings yet
- Sprinter ScheduleDocument1 pageSprinter Schedulepetermcleod1170% (1)
- 2013 Scope of Appointment Form - CORBINDocument2 pages2013 Scope of Appointment Form - CORBINCorbin LindseyNo ratings yet
- FBI NamesDocument5 pagesFBI NamesGrand Jury ActionNo ratings yet
- Draft 1 of Wake County 2022-23 School Enrollment PlanDocument113 pagesDraft 1 of Wake County 2022-23 School Enrollment PlanKeung HuiNo ratings yet
- Healthcare Reimbursement Chapter 3 DiscussionDocument2 pagesHealthcare Reimbursement Chapter 3 Discussionnick5252No ratings yet
- Training MateriaL RCM (Healthcare)Document66 pagesTraining MateriaL RCM (Healthcare)Naveen Babu100% (1)
- Delmar Mounts SSNDOBDocument5 pagesDelmar Mounts SSNDOBtruongcongtuananh100% (1)
- Obama SSN Fraud ProofDocument10 pagesObama SSN Fraud ProofPamela Barnett0% (1)
- Healthcare Common Procedural Coding SystemDocument4 pagesHealthcare Common Procedural Coding SystemTherese WilliamsNo ratings yet
- 07 BpqyDocument1 page07 BpqyMichael Van EssenNo ratings yet
- Medicare and BTGC 2014Document4 pagesMedicare and BTGC 2014Todd GroveNo ratings yet
- AHM 250 SummaryDocument116 pagesAHM 250 SummarySanthosh KumarNo ratings yet
- Medicare BookletDocument152 pagesMedicare BookletMegan KelleyNo ratings yet
- Feb 2017 Final ReportDocument64 pagesFeb 2017 Final ReportSHADACNo ratings yet
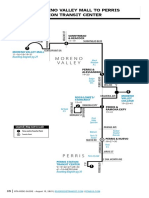
- Route 19 From Perris - Moreno ValleyDocument5 pagesRoute 19 From Perris - Moreno ValleyBenson TautalaNo ratings yet
- Van Buren Township Police Dispatch LogsDocument35 pagesVan Buren Township Police Dispatch LogsAusten SmithNo ratings yet
- 2016 New Medicare Shared Savings Pogram ACOsDocument19 pages2016 New Medicare Shared Savings Pogram ACOsiggybauNo ratings yet
- Authorization For Reimbursement of Interim Assistance Initial Claim or Posteligibility Case SSP 14Document2 pagesAuthorization For Reimbursement of Interim Assistance Initial Claim or Posteligibility Case SSP 14Harry TajyarNo ratings yet
- 16-20 SOCIAL SECURITY NUMBER REQUIREMENT (1) - NQwjuxl (2) .pdf6502326d1291b53320Document13 pages16-20 SOCIAL SECURITY NUMBER REQUIREMENT (1) - NQwjuxl (2) .pdf6502326d1291b53320ElfawizzyNo ratings yet
- 7b MapDocument1 page7b MapAnonymous Pb39klJNo ratings yet
- Sounder Train Schedules: Lakewood To Seattle (Northbound)Document2 pagesSounder Train Schedules: Lakewood To Seattle (Northbound)Mason McCormickNo ratings yet
- Status Report For DMDocument111 pagesStatus Report For DMGanesh KumarNo ratings yet
- AASHTO T324-Hamburg Wheel Tracking TestDocument10 pagesAASHTO T324-Hamburg Wheel Tracking TestTamanna KabirNo ratings yet
- Fema CertificationDocument1 pageFema Certificationapi-365744485No ratings yet
- Impact of Medicaid Extension and Local Spending For Health Care by Texas Senate DistrictDocument62 pagesImpact of Medicaid Extension and Local Spending For Health Care by Texas Senate Districtbee5834No ratings yet
- RA MEDTECH TUGUE Mar2018 PDFDocument11 pagesRA MEDTECH TUGUE Mar2018 PDFPhilBoardResultsNo ratings yet
- BCBS Provider ManualDocument40 pagesBCBS Provider Manualnetgazer79No ratings yet
- Swat Tactic ManualDocument141 pagesSwat Tactic ManualJ_Klaus94% (16)
- The NY-NJ Regional Transit MapDocument1 pageThe NY-NJ Regional Transit MapkatehindsNo ratings yet
- Lavoy Finicum Autopsy ReportDocument13 pagesLavoy Finicum Autopsy ReportJack Ryan100% (3)