Professional Documents
Culture Documents
Tetralogy of Fallot
Uploaded by
Maria Visitacion0 ratings0% found this document useful (0 votes)
180 views26 pagesTetralogy of fallot
Original Title
Tetralogy of fallot
Copyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentTetralogy of fallot
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
180 views26 pagesTetralogy of Fallot
Uploaded by
Maria VisitacionTetralogy of fallot
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You are on page 1of 26
Tetralogy of Fallot
Tetralogy of Fallot is a type of congenital heart defect. Congenital
means that it is present at birth.
Causes
Tetralogy of Fallot causes low oxygen levels in the blood. This leads
to cyanosis (a bluish-purple color to the skin).
Factors that increase the risk for this condition during pregnancy
include:
Alcoholism in the mother
Diabetes
Mother who is over 40 years old
Poor nutrition during pregnancy
Rubella or other viral illnesses during pregnancy
Symptoms
Blue color to the skin (cyanosis), which gets
worse when the baby is upset
Clubbing of fingers (skin or bone enlargement
around the fingernails)
Difficulty feeding (poor feeding habits)
Failure to gain weight
Passing out
Poor development
Squatting during episodes of cyanosis
Exams and Tests
A physical examination with a stethoscope almost
always reveals a heart murmur.
Tests may include:
Chest x-ray
Complete blood count (CBC)
Echocardiogram
Electrocardiogram (EKG)
MRI of the heart (generally after surgery)
Most cases can be corrected with surgery. Babies who
have surgery usually do well. More than 90% survive to
adulthood and live active, healthy, and productive lives.
Without surgery, death usually occurs by the time the
person reaches age 20.
Treatment
Surgery to repair tetralogy of Fallot is done when
the infant is very young. Sometimes more than
one surgery is needed. When more than one
surgery is used, the first surgery is done to help
increase blood flow to the lungs.
Surgery to correct the problem may be done at a
later time. Often only one corrective surgery is
performed in the first few months of life.
Corrective surgery is done to widen part of the
narrowed pulmonary tract and close the
ventricular septal defect.
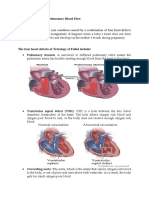
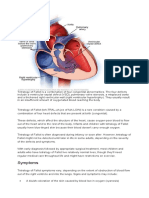
Tetralogy of Fallot is a birth defect of the heart consisting of four abnormalities
that results in insufficiently oxygenated blood pumped to the body. It is classified
as a cyanotic heart defect because the condition leads to cyanosis, a bluish-purple
coloration to the skin, and shortness of breath due to low oxygen levels in the
blood. Surgery to repair the defects in the heart is usually performed between 3
and 5 years old. In more severe forms, surgery may be indicated earlier. In most
cases the heart can be surgically corrected and the outcome is good.
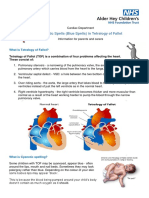
Tet spells
Sometimes, babies with tetralogy of Fallot will suddenly
develop deep blue skin, nails and lips after crying,
feeding, having a bowel movement, or kicking his or her
legs upon awakening. These episodes are called Tet
spells and are caused by a rapid drop in the amount of
oxygen in the blood. Toddlers or older children may
instinctively squat when they are short of breath.
Squatting increases blood flow to the lungs. Tet spells
are more common in young infants, around 2 to 4
months old.
Pulmonary valve stenosis. This is a narrowing of the
pulmonary valve, the flap that separates the right
ventricle of the heart from the pulmonary artery, the main
blood vessel leading to the lungs. Constriction of the
pulmonary valve reduces blood flow to the lungs. The
narrowing may also affect the muscle beneath the
pulmonary valve.
Ventricular septal defect. This is a hole in the wall that
separates the two lower chambers (ventricles) of the
heart. The hole allows deoxygenated blood in the right
ventricle blood that has circulated through the body
and is en route to the lungs to replenish its oxygen
supply to flow into the left ventricle and mix with
oxygenated blood fresh from the lungs. Blood from the
left ventricle also flows back to the right ventricle in an
inefficient manner. This ability for blood to flow through
the ventricular septal defect dilutes the supply of
oxygenated blood to the body and eventually can
weaken the heart.
Overriding aorta. Normally the aorta, the main artery
leading out to the body, branches off the left ventricle. In
tetralogy of Fallot, the aorta is shifted slightly to the right
and lies directly above the ventricular septal defect. In
this position the aorta receives blood from both the right
and left ventricles, mixing the oxygen-poor blood from
the right ventricle with the oxygen-rich blood from the left
ventricle.
Right ventricular hypertrophy. When the heart's
pumping action is overworked, it causes the muscular
wall of the right ventricle to enlarge and thicken. Over
time this may cause the heart to stiffen, become weak
and eventually fail.
Rarely, some babies who have tetralogy of Fallot will
have a hole between their heart's upper chambers (atrial
septal defect), as well. When this occurs, the condition is
known as pentalogy of Fallot.
Patent ductus arteriosus
Patent ductus arteriosus (PDA) is a condition in which
the ductus arteriosus does not close. (The word "patent"
means open.)
The ductus arteriosus is a blood vessel that allows blood
to go around the baby's lungs before birth. Soon after the
infant is born and the lungs fill with air, the ductus
arteriosus is no longer needed. It usually closes in a
couple of days after birth.
PDA leads to abnormal blood flow between the aorta
and pulmonary artery, two major blood vessels that carry
blood from the heart.
PDA affects girls more often than boys. The
condition is more common in premature infants
and those with neonatal respiratory distress
syndrome. Infants with genetic disorders, such
as Down syndrome, and whose mothers had
rubella during pregnancy are at higher risk for
PDA.
PDA is common in babies with congenital heart
problems, such as hypoplastic left heart
syndrome, transposition of the great vessels,
and pulmonary stenosis.
Symptoms
A small PDA may not cause any symptoms.
However, some infants may have symptoms
such as:
Fast breathing
Poor feeding habits
Rapid pulse
Shortness of breath
Sweating while feeding
Tiring very easily
Poor growth
keeping the ductus arteriosus open may be lifesaving.
Medicine may be used to stop it from closing.
When treatment is needed, medications such as
indomethacin or a special form of ibuprofen are often the
first choice. Medicines can work very well for some
newborns, with few side effects. The earlier treatment is
given, the more likely it is to succeed.
If a small PDA stays open, the baby may eventually
develop heart symptoms. Babies with a larger PDA could
develop heart problems such as heart failure, high blood
pressure in the arteries of the lungs, or an infection of
the inner lining of the heart if the PDA does not close.
CAUSES
As a baby develops in the womb, a vascular connection (ductus
arteriosus) between two major blood vessels leading from the heart
the aorta and pulmonary artery is a normal and necessary part
of your baby's blood circulation while in the womb. The ductus
arteriosus diverts blood from the lungs of the fetus while they aren't
being used. The fetus receives oxygen from the mother's circulation.
But, the ductus arteriosus is supposed to close within two or three
days after birth once the newborn's heart adapts to life outside the
womb. In premature infants, the connection often takes longer to
close on its own. If the connection remains open, it's referred to as a
patent ductus arteriosus.
The abnormal opening causes too much blood to circulate to the
lungs and heart. If not treated, the blood pressure in the lungs may
increase (pulmonary hypertension) and the heart may enlarge and
weaken.
Congenital heart defects arise from problems early in the heart's
development but there's often no clear cause. Genetics and
environmental factors may play a role.
The heart pumps blood throughout
the body. It is located in the thorax.
The type and timing of surgical repair depends on the child's condition and the type and
severity of heart defects.
In general, symptoms that indicate that surgery is needed are:
difficulty breathing because the lungs are wet, congested, or fluid-filled (congestive heart
failure)
problems with heart rate or rhythm (arrhythmias)
excessive work load on heart that interferes with breathing, feeding, or sleeping
An incision may be made through the breastbone (sternum) and
between the lungs (mediastinum) while the child is deep asleep and
pain-free (under general anesthesia). For some heart defect repairs,
the incision is made on the side of the chest, between the ribs
(thoracotomy) instead of through the breastbone. Heart-lung bypass
may be needed. Tubes are used to re-route the blood through a special
pump that adds oxygen to the blood and keeps it warm and moving
through the rest of the body while the repair is being done.
Most children need to stay in the Intensive Care Unit for 3 to 7 days
and stay in the hospital for 5 to 14 days. By the time the child is
transferred out of the intensive care unit, most of the tubes and wires
have been removed and he is encouraged to resume many of his daily
activities. At the time of discharge, the parents are instructed on
activity, how to care for the incision and how to give medications their
child may need to take such as Digoxin, Lasix, Aldactone and
Coumadin. The child needs at least several more weeks at home to
recover.
Risk factors for having a patent ductus arteriosus include:
Being born too soon (premature). Patent ductus arteriosus (PDA)
occurs more commonly in babies who are born too early than in babies
who are born full term.
Having other heart defects. Babies who have other heart problems
when they're born (congenital heart defects) are also more likely to
have a patent ductus arteriosus.
Family history and other genetic conditions. If you have a family
history of heart defects, it's more likely your child may have a patent
ductus arteriosus. Other genetic conditions, such as Down syndrome,
also have been linked to an increased chance of having a PDA.
Rubella infection during pregnancy. Becoming infected with rubella
(German measles) while pregnant can increase the risk of heart
defects. The rubella virus crosses the placenta and spreads through
the baby's circulatory system damaging blood vessels and organs,
including the heart.
Having a female baby. PDAs are much more common in girls than in
boys.
Being born at a high altitude. Babies born above 10,000 feet (3,048
meters) have a greater risk of a PDA than babies born at lower
altitudes.
Ventricular septal defect
Ventricular septal defect describes one or more
holes in the wall that separates the right and left
ventricles of the heart. Ventricular septal defect
is one of the most common congenital (present
from birth) heart defects. It may occur by itself or
with other congenital diseases.
Causes
Before a baby is born, the right and left ventricles of its heart are not
separate. As the fetus grows, a wall forms to separate these two ventricles.
If the wall does not completely form, a hole remains. This hole is known as
a ventricular septal defect, or a VSD.
Ventricular septal defect is one of the most common congenital heart
defects. The baby may have no symptoms, and the hole can eventually
close as the wall continues to grow after birth. If the hole is large, too much
blood will be pumped to the lungs, leading to heart failure.
The cause of VSD is not yet known. This defect often occurs along with
other congenital heart defects.
In adults, ventricular septal defects are a rare but serious complication of
heart attacks. These holes do not result from a birth defect.
A ventricular septal defect occurs when the septum, the
muscular wall separating the heart into left and right
sides, fails to form fully between the lower chambers of
the heart (ventricles) during fetal development. This
leaves an opening that allows mixing of oxygenated
blood and deoxygenated blood, meaning the heart has
to work harder to provide enough oxygen to your body's
tissues.
If a ventricular septal defect is large, blood overfills the
lungs and overworks the heart. If left untreated, the
blood pressure in the lungs goes up (pulmonary
hypertension) and the ventricles enlarge and no longer
work efficiently. Ultimately, this can lead to irreversible
damage to the lung arteries and to heart failure. In
contrast, small ventricular septal defects don't usually
cause any problems, except for a loud heart murmur that
doctors may note during physical exams.
Symptoms
Patients with ventricular septal defects may not have
symptoms. However, if the hole is large, the baby often
has symptoms related to heart failure.
The most common symptoms include:
Shortness of breath
Fast breathing
Hard breathing
Paleness
Failure to gain weight
Fast heart rate
Sweating while feeding
Frequent respiratory infections
Exams and Tests
Listening with a stethoscope usually reveals a heart
murmur (the sound of the blood crossing the hole). The
loudness of the murmur is related to the size of the
defect and amount of blood crossing the defect.
Tests may include:
Cardiac catheterization (rarely needed, unless there are
concerns of high blood pressure in the lungs)
Chest x-ray -- looks to see if there is a large heart with
fluid in the lungs
ECG -- shows signs of an enlarged left ventricle
Echocardiogram -- used to make a definite diagnosis
MRI of the heart -- used to find out how much blood is
getting to the lungs
Treatment
If the defect is small, no treatment is usually needed. However, the
baby should be closely monitored by a health care provider to make
sure that the hole eventually closes properly and signs of heart
failure do not occur.
Babies with a large VSD who have symptoms related to heart failure
may need medicine to control the symptoms and surgery to close
the hole. Medications may include digitalis (digoxin) and diuretics.
If symptoms continue even with medication, surgery to close the
defect with a Gore-tex patch is needed. Some VSDs can be closed
with a special device during a cardiac catheterization, although this
is rarely done.
Ventricular septal defect is a congenital defect of the heart, that occurs
as an abnormal opening in the wall that separates the right and left
ventricles. Ventricular septal defect may also be associated with other
heart defects. Many small defects will close on their own. For those
defects that do not spontaneously close, the outcome is good with
surgical repair.
Risk Factors
Ventricular septal defect appears to run in families and
sometimes occurs with other genetic problems, such as Down
syndrome. If you already have a child with a heart defect, a
genetic counselor can predict the approximate odds that your
next child will have one.
Rubella infection. Becoming infected with German measles
(rubella) while pregnant can increase the risk of fetal heart
defects. The rubella virus crosses the placenta and spreads
through the fetus' circulatory system damaging blood vessels
and organs, including the heart.
Poorly controlled diabetes. Uncontrolled diabetes in the
mother in turn affects the fetus' blood sugar, causing
damaging effects to the developing fetus.
Drug or alcohol use or exposure to certain substances. Use
of certain medications, alcohol or drugs or exposure to
chemicals or radiation during pregnancy can harm the
developing fetus.
You might also like
- Tetralogy of FallotDocument9 pagesTetralogy of FallotPaul MagbooNo ratings yet
- Congenital Heart Disease 1223958712449685 9Document58 pagesCongenital Heart Disease 1223958712449685 9RinaNo ratings yet
- LESSON 3. Congenital Heart DefectsDocument9 pagesLESSON 3. Congenital Heart DefectsEdmarie P. TabacoldeNo ratings yet
- Tetralogy of Fallot: Arianna Jasminemabunga Bsn-2BDocument30 pagesTetralogy of Fallot: Arianna Jasminemabunga Bsn-2BArianna Jasmine MabungaNo ratings yet
- Magyawi Tetralogy of Fallot 1st PartDocument7 pagesMagyawi Tetralogy of Fallot 1st PartJoanna Bee Rose MagyawiNo ratings yet
- Tetralogy of FallotDocument33 pagesTetralogy of FallotjeenaejyNo ratings yet
- Patent Ductus Arteriosus (PDA)Document19 pagesPatent Ductus Arteriosus (PDA)putri avriantiNo ratings yet
- Congenital Heart Diseases, A Simple Guide to these Medical ConditionsFrom EverandCongenital Heart Diseases, A Simple Guide to these Medical ConditionsNo ratings yet
- Congenital Heart DefectDocument10 pagesCongenital Heart DefectShubhamNo ratings yet
- Ateneo de Zamboanga University College of Nursing NCM 103 DeliverablesDocument6 pagesAteneo de Zamboanga University College of Nursing NCM 103 DeliverablesNoelle HarrisonNo ratings yet
- Tetraogy of FallotDocument9 pagesTetraogy of FallotMary Louise MadariagaNo ratings yet
- Tetralogy of Fallot: (A Congenital Heart Disease)Document7 pagesTetralogy of Fallot: (A Congenital Heart Disease)Sunil Kumar SahuNo ratings yet
- Tetralogy of FallotDocument3 pagesTetralogy of FallotyasminNo ratings yet
- Tetralogy of FallotDocument5 pagesTetralogy of FallotCharity OaniaNo ratings yet
- Cardiovascular PDFDocument15 pagesCardiovascular PDFGenki Fay B. LequiganNo ratings yet
- Tetralogy of Fallot Lesson PlanDocument25 pagesTetralogy of Fallot Lesson PlanUday Kumar100% (1)
- Tetralogy of Fallot Report 1Document9 pagesTetralogy of Fallot Report 1Maricar EustaquioNo ratings yet
- Child Nursing Care of The High-Risk Newborn To Maturity: I. PrematurityDocument392 pagesChild Nursing Care of The High-Risk Newborn To Maturity: I. PrematuritydaisibanNo ratings yet
- Tetralogy of Fallot Is A Combination of Four Congenital AbnormalitiesDocument4 pagesTetralogy of Fallot Is A Combination of Four Congenital AbnormalitiesJoanne TolopiaNo ratings yet
- What Is A Ventricular Septal DefectDocument2 pagesWhat Is A Ventricular Septal DefectKARAN MOHANANINo ratings yet
- Cyanotic Spells Blue Spells in Tetralogy of Fallot - PIAG 214Document2 pagesCyanotic Spells Blue Spells in Tetralogy of Fallot - PIAG 214imil irsalNo ratings yet
- What Is A Ventricular Septal DefectDocument2 pagesWhat Is A Ventricular Septal DefectKARAN MOHANANINo ratings yet
- Tetralogy of FallotDocument8 pagesTetralogy of FallotHillary Faye FernandezNo ratings yet
- Patent Ductus ArteriosusDocument6 pagesPatent Ductus ArteriosusnidyaparasayuNo ratings yet
- What Is Tetralogy of FallotDocument3 pagesWhat Is Tetralogy of FallotJyedenn PonceNo ratings yet
- Fetal CirculationDocument19 pagesFetal Circulation3sshhhNo ratings yet
- Congenital Heart DiseasesDocument14 pagesCongenital Heart DiseasesEulane Ferrer100% (1)
- 12 - Semiotics of Cardiovascular Disorders. Semiotics of Congenital Hert Diseases in Children.Document30 pages12 - Semiotics of Cardiovascular Disorders. Semiotics of Congenital Hert Diseases in Children.Omowunmi KadriNo ratings yet
- Tetralogy of FallotDocument9 pagesTetralogy of FallotLaurice BarronNo ratings yet
- Congenital Cardiovascular AnomaliesDocument36 pagesCongenital Cardiovascular AnomaliesFauzi SatriaNo ratings yet
- Tetralogy of FallotDocument38 pagesTetralogy of FallotJohn Paul MedalloNo ratings yet
- Tetralogy of FallotDocument7 pagesTetralogy of FallotWidelmark FarrelNo ratings yet
- Ventricular Septal DefectDocument4 pagesVentricular Septal DefectMarina RotaruNo ratings yet
- What Is Tetralogy of Fallot?: Congenital Heart DefectDocument3 pagesWhat Is Tetralogy of Fallot?: Congenital Heart DefectGlenn Asuncion PagaduanNo ratings yet
- Quiz 2 Sa PediaDocument6 pagesQuiz 2 Sa Pediaqweyo yhuNo ratings yet
- Coarctation of The AortaDocument4 pagesCoarctation of The AortaChristine Joy CamachoNo ratings yet
- Cardiovascular System Dr. Eman Badr 2020Document182 pagesCardiovascular System Dr. Eman Badr 2020Amina DinarNo ratings yet
- (Miomio) Maternal-Heart DefectsDocument11 pages(Miomio) Maternal-Heart DefectsJuliet Marie MiomioNo ratings yet
- Explanation Ko ItoDocument5 pagesExplanation Ko ItoJoanna Bee Rose MagyawiNo ratings yet
- Congenital Cardiovascular Anomalies: Dr. Herlina Dimiati, Spa (K)Document36 pagesCongenital Cardiovascular Anomalies: Dr. Herlina Dimiati, Spa (K)EndiRasadiHermanNo ratings yet
- What Is Tetralogy of FallotDocument2 pagesWhat Is Tetralogy of FallotJamaica Cruz San Pedro100% (1)
- Tricuspid AtresiaDocument14 pagesTricuspid AtresiaPretty AjursNo ratings yet
- PAEDs - CVS-1Document44 pagesPAEDs - CVS-1Priscah bhokeNo ratings yet
- Tetralogy of Fallot: What Is It?Document3 pagesTetralogy of Fallot: What Is It?Anditha Namira RSNo ratings yet
- Pathophysiology Congenital Heart Disease-1Document54 pagesPathophysiology Congenital Heart Disease-1single_ladyNo ratings yet
- Tetralogy of Fallot-16 Sept 2014Document21 pagesTetralogy of Fallot-16 Sept 2014aYie_30No ratings yet
- Ventricular Septal DefectDocument6 pagesVentricular Septal DefectYannah Mae EspineliNo ratings yet
- TuGaS Cardi0Document13 pagesTuGaS Cardi0winfrey2207No ratings yet
- Atrial Septal DefectDocument15 pagesAtrial Septal DefectJitendra BhattNo ratings yet
- Embryology of The HeartDocument65 pagesEmbryology of The Heartnisha24No ratings yet
- Pulmonory StenosesDocument9 pagesPulmonory StenosesMaxamed Faarax XaashiNo ratings yet
- Odia Tetralogy of FallotDocument25 pagesOdia Tetralogy of Fallotvictorjonathan567No ratings yet
- Ventricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandVentricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Tetralogy of FallotDocument28 pagesTetralogy of FallotLaurice Grace Zamayla BaelNo ratings yet
- Cardio-Respiratory Conditions: by DR Priscus MushiDocument73 pagesCardio-Respiratory Conditions: by DR Priscus MushiMusaNo ratings yet
- Cardio Pulmonary Resuscitation (CPR) and Automated External Defibrillation (AED) Training GuideFrom EverandCardio Pulmonary Resuscitation (CPR) and Automated External Defibrillation (AED) Training GuideRating: 5 out of 5 stars5/5 (1)
- A Simple Guide to Blood Clot in Lungs, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Blood Clot in Lungs, Diagnosis, Treatment and Related ConditionsNo ratings yet
- Introduction To LeadershipDocument1 pageIntroduction To LeadershipMaria VisitacionNo ratings yet
- UTI IntroDocument1 pageUTI IntroMaria VisitacionNo ratings yet
- 11 Nursing Core ResponsibilityDocument2 pages11 Nursing Core ResponsibilityMaria VisitacionNo ratings yet
- Dar 5Document1 pageDar 5Maria VisitacionNo ratings yet
- Nurse'S Notes (Dar Method)Document1 pageNurse'S Notes (Dar Method)Maria VisitacionNo ratings yet
- DAR Sample 2Document1 pageDAR Sample 2Maria VisitacionNo ratings yet
- DAR SampleDocument1 pageDAR SampleMaria VisitacionNo ratings yet
- Fluids & Electrolyte NewDocument154 pagesFluids & Electrolyte NewMaria Visitacion100% (2)
- BibliographyDocument12 pagesBibliographyMaria VisitacionNo ratings yet
- Brain CancerDocument29 pagesBrain CancerMaria VisitacionNo ratings yet
- Triage 1Document3 pagesTriage 1Maria VisitacionNo ratings yet
- Congenital AnomaliesDocument26 pagesCongenital AnomaliesMaria VisitacionNo ratings yet
- Causes: Polycythemia VeraDocument15 pagesCauses: Polycythemia VeraMaria VisitacionNo ratings yet
- Case FormatDocument12 pagesCase FormatMaria VisitacionNo ratings yet
- Critical Thinking PowerpointDocument16 pagesCritical Thinking PowerpointMaria VisitacionNo ratings yet
- Leukemia ReportDocument5 pagesLeukemia ReportCrisantaCasliNo ratings yet