Professional Documents
Culture Documents
GIT Lecture
Uploaded by
dhainey100%(6)100% found this document useful (6 votes)
2K views93 pagesMost common disorders are reflux esophagitis and carcinoma, both squamous and adenocarcinous being important. The stomach is an important site of peptic ulceration, the ulceration being due to breakdown of the normal mechanisms which protect the stomach mucosa from its own acid. The small intestine, particularly ileum, is the most common site for the chronic inflammatory disease called Crohn's disease.
Original Description:
Copyright
© Attribution Non-Commercial (BY-NC)
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentMost common disorders are reflux esophagitis and carcinoma, both squamous and adenocarcinous being important. The stomach is an important site of peptic ulceration, the ulceration being due to breakdown of the normal mechanisms which protect the stomach mucosa from its own acid. The small intestine, particularly ileum, is the most common site for the chronic inflammatory disease called Crohn's disease.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
100%(6)100% found this document useful (6 votes)
2K views93 pagesGIT Lecture
Uploaded by
dhaineyMost common disorders are reflux esophagitis and carcinoma, both squamous and adenocarcinous being important. The stomach is an important site of peptic ulceration, the ulceration being due to breakdown of the normal mechanisms which protect the stomach mucosa from its own acid. The small intestine, particularly ileum, is the most common site for the chronic inflammatory disease called Crohn's disease.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You are on page 1of 93
Pathology of the oesophagus:
a) disorders of motility, diverticula, varices
b) reflux exophagitis
c) esophageal carcinoma
Pathology of the stomach:
a) gastritis
b) peptic ulcer,
c) tumors - polyps, carcinoma, lymphoma,
stromal tumors.
Appendicitis:
a) acute - morphologic types, evolution, complications
b) chronic - evolution and complications
Pathology of the small and large intestine:
a) vascular disorders
b) inflammatory diseases, infections, enterocolitis
c) Crohn´s disease
d) ulcerative colitis
e) malabsorption syndromes
Pathology of the intestines:
a) neoplasms
b) polyps - non neoplastic, adenomatous - types
c) gastrointestinal polyposis syndromes
d) colorectal carcinoma; lymphomas
e) intestinal lymphomas, stromal tumors
Clinical Overview
Esophagus - most common disorders are reflux esophagitis (due to
exposure of the lower esophagus to gastric acid regurgitating upwards
from the stomach) and carcinoma, both squamous and
adenocarcinoma being important.
In children, esophageal atresia and abnormal developmental links with
the trachea are important congenital malformations.
The stomach is an important site of peptic ulceration, the ulceration
being due to breakdown of the normal mechanisms which protect the
stomach mucosa from its own acid.
The small intestine is the major site of absorption of the basic food
materials, and diseases of small intestinal mucosa may lead to
malabsorption syndromes; an important cause is celiac disease
(gluten enteropathy) which is an immune process leading to destruction
of the small intestinal mucosa.
The small intestine, particularly ileum, is the most common site for the
chronic inflammatory disease called Crohn’s disease.
Acute inflammatory disorders of the small bowel are common but
transient, being due to bacterial or viral infection. The stomach and
colon are usually also involved (infective gastroenteritis).
Most common inflammatory disease of the entire alimentary tract which
requires surgical treatment is acute appendicitis, mainly in children and
young adults, but occasionally in mature adults and the elderly where the
diagnosis may be missed.
The colon may also be involved in the chronic inflammatory condition
Crohn’s disease, but is the main site of the chronic intermittent
inflammatory disease called ulcerative colitis.
Predisposing factors to colonic cancer - neoplastic polyps in the colonic
mucosa (adenomatous polyps).
Colorectal carcinoma there is a well-recognized sequence of
changes from benign polyp to invasive adenocarcinoma.
Colon - mechanical abnormalities diverticular disease and volvulus.
Disorders of the anus are a frequent are mainly trivial with distressing
symptoms (hemorrhoids, pruritus ani, anal fissure); the only life-
threatening disease of the anus is squamous carcinoma.
GIT is susceptible to bacterial and viral infection, producing acute
vomiting and diarrhea, the main source for the infection being
contaminated or infected food items (‘food poisoning’).
Vascular diseases affecting the alimentary tract are uncommon,
with the exception of arterial infarction of the small bowel due to
thrombotic or embolic occlusion of the mesenteric vessel, and
acute venous infarction of small or large bowel due to some
mechanical obstruction to normal venous drainage.
The most common examples of venous infarction of the bowel are
strangulation of a loop of small bowel in a hernial sac and
volvulus of the large bowel.
Esophagus
Lesions – esophagitis to cancer
Dysphagia (difficulty in swallowing)
esophageal motor dysfunction,
Narrowing, or obstruction
Clinical manifestations
6.Heartburn (retrosternal burning pain) –
regurgitation of gastric contents
7.Hematemesis
8.Melena
Esophagus
Anatomic disorders of the esophagus
1.Stenosis- lower esophageal narrowing,
chronic inflammation, GERD
2.Atresia, fistula- newborn with
aspiration, paroxysmal suffocation,
pneumonia (tracheoesophageal fistula)
3.Webs, rings- dysphagia to solid foods,
partially occluding lumen
4.Diverticula- nocturnal episodic
regurgitation
Hiatal hernia- dilated segment
of the stomach to protrude
above the diaphragm
Sliding- 95% of cases, 9% with
heartburn (accentuated by
bending forward, supine
position, obesity)
Paraeophageal- separate
portion of the stomach
enters the thorax through
a widened foramen, rarely
with reflux, can become
strangulated/ obstructed
Complications- ulceration,
bleeding, perforation
Esophagus
Achalasia- incomplete relaxation of the lower
esophageal sphincter to relax during swallowing:
2. Aperistalsis
3. Incomplete relaxation
4. Increased resting tone
Primary- loss of intrinsic inhibitory innervation of the
lower esophageal sphincter and smooth muscle
segment
Secondary- Chagas disease (Trypanosoma cruzi)
-myenteric plexus of the GIT
Other possible causes- autoimmunity, previous
viral infection (unproven)
5% cases result to CA
Esophagus
Lacerations (Mallory-Weiss syndrome)
Longitudinal tear esophagogastric junction
Severe vomiting/ retching – alcoholics/ acute
illness
Pathogenesis- incomplete relaxation of the
esophageal sphincter during vomiting
Tearing of the involved area
75% cases have hiatal hernia
Tears may involve mucosa or penetrate the wall,
infection may lead to an inflammatory
ulceration/ mediastinitis
(5 to 10% of upper GI bleeding due to
esophageal laceration)
Esophagus
Varices- dilated tortuous vessels, due to
collateral by-pass channels caused by
cirrhosis, 2/3 of cases, no symptoms
until they rupture
Cause of rupture – unclear, possibly
erosion of the mucosa, increased
tension, vomiting
50% with concomittant liver CA
50% cases subsides spontaneously
Mortality – 20 to 30%
Esophagus
Esophagitis-
Prolonged gastric intubation
Uremia
Corrosive/ irritant substances
Radiation or chemotheraphy
Major cause – gastroesophageal reflux disease
(0.5% of adult American)
Heartburn is a predominant symptom
Contributory factors
10.Less effective anti-reflux mechanisms
11.Inadequate clearance of refluxed material
12.Sliding hiatal hernia
13.Increased gastric volume
14.Reduced reparative capacity – prolonged exposure to
gastric juices
Esophagus
Esophagitis-
Morphology
Mild- simple hyperemia
Severe- erosion or total ulceration
Characteristics of uncomplicated Reflux
esophagitis
6. Epithelial layer with eosinophil with or without
neutrophil
7. Basal zone hyperplasia
8. Elongation of lamina propria papillae
CM – heartburn, chest pain may mimic heart
attack
Sequelae- bleeding, stricture, Barrett esophagus
Esophagus
Barrett esophagus- complication of a long-
standing GERD
Up to 10% of patients with persistent symptomatic
reflux disease
-replacement of the distal stratified squamous
mucosa by metaplastic columnar epithelium
containing goblet cells (more resistant to gastric
content)
male: female ratio = 4:1, common among whites
Complications
6. Ulcer, stricture
7. Cancer – 30 to 40-fold increase
Esophagus
Esophageal CA
Squamous CA- 90% of cases, > age 50, male:female ratio 3:1
Adenocarcinoma- increasing incidence, more among whites
Morphology
Early – small gray-white thickening or elevation of the mucosa
3 types
7. exophytic, protrude into lumen
8. Necrotizing, erodes into the respiratory tree, aorta, elsewhere
9. Diffuse infiltrative
Involvement
Cervical- 20%
Middle third – 50%
Lower third – 30%
Esophagus
Esophageal CA
Adenoca
-arise from dysplastic mucosa of Barrett esophagus
Usually in the distal third
Micros- mucin-producing glandular tumor
CM
Insidous onset, dysphagia and obstruction
-weight loss, anorexia, fatigue, weakness
-pain related to swallowing
Surgical excision is rarely curative – lymphatic
network, adjacent structure
Amenable to surgery if confined to mucosa or submucosa
Stomach
Chronic gastritis
-chronic mucosal inflammatory changes lead to mucosal
atrophy and epithelial metaplasia
-Helicobacter pylori- non-invasive non-spore forming gram
negative rod, bacterial enzymes and toxins, release of
chemicals by recruited neutrophil
-autoimmune gastritis- gland destruction and mucosal
atrophy,
loss of parietal cells
Morphology- chronic gastritis- inflammatory changes consist
of lymphocytic and plasma cell infiltrate in the lamina propria
with variable gland loss and mucosal atrophy
CM- few or no symptoms, upper abdominal discomfort, n/v
Most patients with peptic ulcer have H. pylori infections,
risk for gastric CA 5X
Autoimmune gastritis, risk for cancer from 2% to 4%
Stomach
Acute gastritis
-acute mucosal inflammatory process, usually
of transient nature, may be accompanied by
bleeding and mucosal erosion
Pathogenesis
-NSAID(aspirin)
Excessive alcohol intake, heavy smoking
Anti-cancer drugs
Uremia
Systemic infection (typhoid fever)
Severe stress (trauma, burns, surgery)
Ischemia and shock
Suicide using acid or alkali
Mechanical trauma (NGT)
Stomach
Acute gastritis
Morphology- localized to diffused involvement,
superficial inflammation of the entire mucosa thickness,
with bleeding and erosion (acute erosive gastritis)
If the noxious event is short lived – complete recovery of
the mucosa
CM- asymptomatic, epigastric pain with N/V,
hematemesis, melena, possible fatal blood loss
-major cause of hematemesis (alcoholics)
-25% of patients taking aspirin for RA develop acute
gastritis
Gastric ulceration
Breach in the mucosa, could extend to muscularis
mucosae into submucosa or deeper
Stomach
Peptic ulcers
-chronic, often solitary, due to aggressive action of
acid-peptic juices
98% in the first portion of duodenum or stomach
(ratio 4:1)
American- 2.5% males, 1.5% females
Genetic or racial factors- plays no role in its causation
Duodenal ulcers- alcoholic cirrhosis, COPD, chronic
renal disease, hyperparathyroidism
(hypercalcemia stimulate gastrin production)
Pathogenesis
10.Mucosal exposure to gastric acid and pepsin
11.H. pylori infection
Actual pathogenesis is murky
Stomach
Peptic ulcers
Host mechanism that protects the
mucosa from gastric juices
3.Mucus – superficial epithelial cells
4.Bicarbonate secretion
5.Acid and pepsin secreted as “jets”
6.Epithelial regeneration
7.Robust mucosal blood flow
8.Mucosal prostaglandins – maintain
blood flow
Stomach
H. Pylori
70% to 90%- patients with duodenal ulcer
70% - gastric ulcers
-induce inflammatory and immune
response
-produce urease (toxin),
phospholipase (mucosal damage)
-vacuolating toxin (VacA), cytotoxin-assod
gene A (CagA)- secretes IL-8 -recruits
and activates neutrophils
Stomach
Peptic ulcers
NSAID- second to H. pylori
Risk factors – increasing age, higher dose,
prolonged use
-suppress mucosal prostraglandin synthesis
(more acid, less mucus and less bicarbonate)
-impairs angiogenesis- impedes healing of
ulcers
Others
7. Smoking- mucosal blood flow, healing
8. Alcohol – directly cause PU
9. Stress
10.Zollinger-Ellison syndrome
(multiple peptic ulcers - gastrin secretion by a tumor)
Stomach
Peptic ulcer
Morphology
Mucosal defects that penetrates deeper, mostly round,
sharply punched out craters 2 to 4 cm.
Sites- ant and post wall duodenum, lesser curvature
No significant elevation or beading of the edges
Micros- vary with activity, chronicity, degree of healing
Diff from AGU- absent gastritis in adjacent mucosa
CM- epigastric gnawing, burning, boring pain, worse at
night, occurs 1 to 3 hours after meals
Relieve by alkali or food (there are many exceptions)
Other- n/v, bloating, belching, weight loss
Bleeding- chief complication, perforation, malignant transformation
PU- chronic and recurrent, impairs quality of life than
shorten it Requires 15 years for healing
Stomach
Stomach
Acute gastric ulceration
Stress ulceration- multiple lesions
• Severe trauma (surgical procedures, sepsis, grave
illness
• Extensive burns (Curling ulcers)
• Traumatic or surgical injury to the CNS, or
intracerebral bleeding (Cushing ulcers)
Pathogenesis – uncertain – systemic acidosis (severe trauma and
burns)- decrease pH of mucosal cells, hypoxia, impaired
mucosal blood flow
Cranial lesion – increase ICP stimulate vagal nuclei – increased
acid secretion
Morphology – circular and small (less than 1 cm), base dark brown,
singly to multiple throughout stomach and duodenum
CM- ICU admitted patients with sepsis, burns or trauma dev AGU
Treatment- prophylactic antacid, blood transfusion
Need to correct the underlying condition
Gastric mucosa can recover completely if the patient does not die.
Stomach
TUMORS
Gastric polyps- mass or nodule that project
above the level of the surrounding mucosa,
these are uncommon
Types
4. Hyperplastic – 80% to 85%
5. Fundic gland – 10%
6. Adenomatous – 5%
All arise from a setting of chronic gastritis –
adematous polyp has a risk of containing
an adenoCA
Stomach
TUMORS
Gastric Carcinoma
Carcinoma – 90% to 95%
Lymphomas – 4%
Carcinoid – 3%
Mesenchymal spindle cell tumor – 2%
High incident – Japan, columbia, Costa Rica, Hungary
One of the leading killer cancer
Morphology- intestinal (gastric mucous cells that have
undergone metaplastic dysplasia in the setting of
chronic gastritis, better differentiation)
Common type in high risk population,
occurs after age 50 years with 2:1 male predominance
Diffuse variant arise from gastric mucous cells, not
associated with chronic gastritis
Poorly differentiated, earlier age, no male predominance
Stomach
Gastric Cancer
Morphology
Site
1. Pylorus and antrum – 50% to 60%
2. Cardia – 25%
3. Body and fundus – 12%
4. Lesser curvature – 40%
5. Greater curvature – 12%
*ulcerative lesion on the lesser curvature – more likely malignant
Classification
1. Depth of invasion
2. Macroscopic growth pattern
3. Histologic subtype
Gastric Cancer
Morphology
Depth of invasion –
morphologic feature
having the greatest impact
on clinical outcome
Early GC – lesion confined to
the mucosa and
submucosa, regardless of
the presence
or absence of of
perigastric LN
Advanced GC – extended
below the submucosa into
the muscular wall
*Mucosal dysplasia precursor lesion
Gastric Cancer
Morphology
Uncommon, a broad area of the gastric wall, or entire
stomach, extensive infiltration, rigid and thickened
stomach is termed a leather bottle stomach
-linitis plastica, metastatic ca from the breast and lung
may generate a similar picture
The earliest LN metastasis may sometimes involve a
supraclavicular LN (Virchow’s node)
Unusual intraperitoneal spread to both ovaries – Krukenberg
tumor
CM- early is asymptomatic, advanced – may be
asymptomatic, abdominal discomfort or weight loss
Only hope for cure is early detection and surgical removal
Prognostic indicator – stage of tumor at the time of resection
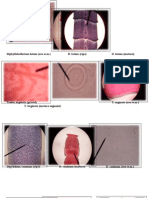
Gastric Ca- signet ring
Small and Large Intestines
Developmental anomalies
2. Atresia, stenosis
3. Duplication
4. Meckel’s diverticulum- failure of involution of
omphalomesenteric duct leaving a persistent
blind-ended tubular protrusion 5 to 6 cm long
5. Omphalocele- congenital defect of the
periumbilical abdominal wall, membranous
sac in which the intestines herniate
6. Malrotation- intestines not in their normal
position
7. Hirschsprung disease leading to congenital
megacolon
Small and Large Intestines
Developmental anomalies
Hirschsprung disease leading to congenital
megacolon- aganglionic segment
Lacks Meissner submucosal, Auerbach myenteric
plexuses.
Functional obstruction, distension of the colon
proximal to the affected segment
CM- delay in the initial passage of meconium,
followed by vomiting 48 to 7 hours
Enterocolitis, fluid and electrolyte imbalance, perforation
Acquired megacolon
• Chaga’s disease –trypanosomes
• Obstruction by neoplasm, inflammatory stricture
• Toxic megacolon complicating CD or UC
Small and Large Intestines
VASCULAR DISORDER
Ischemic bowel disease
Intensive infarction – occlusion of any of the major arteries-
celiac, superior and inferior mesenteric arteries
Transmural – acute occlusion of the major mesenteric
artery
Mural or mucosal – physiologic hypoperfusion, localized
anatomic defect
Predisposing factors
8. Arterial thrombosis – severe atherosclerosis, dissecting aneurysm, systemic
vasculitis,
9. Angiographic procedures, aortic surgery, surgical accidents, hypercoagulable disorder
10. Oral contraceptives
11. Arterial embolism- cardiac vegetation, aortic atheroembolism
12. Venous thrombosis- hypercoagulable state-oral contraceptives, intraperitoneal sepsis
13. Post-op state hepatocellular CA, cirrhosis, abdominal trauma
14. Nonocclusive ischemia- CF, shock, dehydration, vasoconstrictive drugs
(digitalis,vasopresin, propanolol)
15. Others- radiation injury, volvulus, stricture, herniation
CM- most common in the later years of life,
transmural sudden onset of abdominal pain,
sometimes with bloody diarrhea,
need for prompt diagnosis
(recent major abdominal surgery, recent MI,
atrial fib)
mortality rate = 90%
Diarrheal diseases
-increase stool mass,
stool frequency,
stool fluidity,
often with pain, urgency,
perianal discomfort,
incontinence
Dysentery- low volume,
painful, bloody diarrhea
Malabsorption
Gluten-sensitive enteropathy- Celiac disease- reduced small
intestinal absorptive
Surface area- sensitivity to gluten (oat, barley, rye)
immune response- damage to surface enterocyte
-symptomatic diarrhea and malnutrition from infancy to mid-
adulthood,
Removal of gluten in diet results in dramatic improvement
Tropical sprue, whipple disease- arise from intestinal infection
results in celiac-like disease within few days after acute diarrheal
enteric infection
-rare, affects intestine, CNS, joint. Hallmark PAS-positive
macrophages in the lamina propria. Etio-gram + and culture R
actinomycete (tropheryma whippelli) males, 4th to 5th decades of
life-
-malabsorption, lymphadenopathy, hyperpigmentation,
polyarthritis, obscure CNS complaints
CM- bulky frothy, greasy, yellow or gray stool with weight loss,
anorexia, Abdominal distention, borborygmi, flatus, muscle
wasting
Consequences of malabsorption
IDIOPATHIC INFLAMMATORY BOWEL
DISEASE
Crohn disease, ulcerative colitis
Chronic relapsing disorders of unknown origin
Collectively called IBD.
Normal intestine represents adynamic balance between
6. Factors that activate the host immune system –such as
luminal microbes, dietary antigens, endogenous
inflammatory stimuli
7. Host defenses that down regulate inflammatory and
maintain integrity of the mucosa
IBD is a heterorogenous group of diseases characterized
by exaggerated destructive mucosal immune response.
Tissue injury is likely to be initiated by diverse genetic and
immunologic
pathways that are modified by environmental influences,
including microbes and their products
CROHN DISEASE
Involves any level of the GIT, associated with complication
of immune origin like iritis, uveitis, migratory polyarthritis,
it is a systemic inflammatory disease with predominant
GIT involvement, peaks 2nd to 3rd decade of life, more
among women, whites, Jews
Characterized by transmural involvement with mucosal
damage, caseating granuloma 40% to 60% cases,
fissuring and fistulae, sinus tract formation. Thick and
rubbery wall. “string sign”. Skip lesion. Microscopic-
inflammation, crypt abscess, ulceration, chronic mucosal
damage.
CM- variable presentation, recurrent diarrhea, crampy abdominal pain,
fever lasting days to weeks, melena- 50%, 10-20% symptom free for
decades after initial attacks, 20% continuous active disease
Complications- fistula, abdominal abscess, strictures/ obstruction
Rare- massive intestinal bleeding, toxic dilatation of colon, cancer
ULCERATIVE COLITIS
ulceroinflammatory disease – colon, limited to the mucosa
and submucosa except in severe cases, begins in
rectum
Epidemiology- more common than CD, whites, no sex
predilection, peaks at age 20 to 25
Morphology- involves rectum or rectosigmoid colon only in
50% of cases, pseudopolyps- isolated islands of
regenerating mucosa
Pathologic features- mucosal inflammation, ulceration,
chronic mucosal damage
1.Mononuclear infiltrate 2.ulceration 3. granulation tissue
4.submucosal fibrosis and mucosal atrophy
CM- relapsing and remitting disorder- bloody mucoid
diarrhea persists for days, weeks, months. Insidious,
cramp, tenesmus, colicky abdominal pain relieved by
defecation. Fever, weight loss. 10% first attack is the last
ULCERATIVE COLITIS
Colonic diverticulosis
Diverticulum- uncommon
Blind pouch leaving off the gut, lined by a mucosa.
Most diverticulitis are acquired, lacking or having
attenuated muscularis propria.
Common site for diverculum- colon,
diverticular disease of the colon -diverticulosis
Common among western adults, prevalence is about
50% by age 60
-low fiber diet, reduced stool bulk, exaggerated spastic
contraction- herniation of the bowel wall
Pathogenesis
1.Exaggerated peristaltic contractions- increase
intraluminal pressure
2.Focal defect in the muscular colonic wall
Bowel obstruction
80% of cases due to; hernias, intestinal adhesions,
intussusception, volvulus (small intestines commonly involve
due to its small lumen)
Hernial sac- protrusion of a pouch-like sac through a
weakness or defects in the abdominal cavity
Usual sites anteriorly
1.Inguinal and femoral canals
2.Umbilicus
3.Surgical scar
Incarceration- permanently trapped
Strangulation- infarction due to compromised blood supply
Adhesions-surgery, infection, endometriosis- intestine are
trapped (internal hernia)
Intussusception- telescoping of proximal segment into a immediately distal
segment - Common in children may be due to excessive peristaltic activity.
Adults- Intraluminal mass (tumor)- infarction
Volvulus- twisting of bowel loops about its base of
attachment- small intestines
Small and Large Intestines
Tumors
Epithelial tumors of the intestines are major causes of
diseases and death worldwide
Colorectal cancer second only to bronchogenic
carcinoma among the cancer killers
About 5% Americans will develop colorectal cancer,
40% of them will die of the disease
Adenocarcinoma most common colorectal cancer
accounts for 70% of all GIT malignancy.
Small intestine uncommon site for tumor,
Polyp- mass protrudes into the lumen- 1. pedunculated,
(stalk) 2. sessile
-formed by abnormal mucosal maturation, inflammation,
architecture
No malignancy potential (hyperplastic polyp)
-those that arise due to epithelial proliferation and dysplasia
(adenomatous polyp or adenoma)
Precursor of cancer
Tumors of the small and large intestines
Benign
Hyperplastic polyp
Hamartomatous polyp
Inflammatory polyp
Lymphoid polyp
Neoplastic-epithelial lesions
Benign polyps – adenoma
Malignant lesions – adenoCA,
carcinoid tumor, angioma
Mesenchymal lesions
Gastrointestinal stromal tumors (benign or malignant)
Other benign lesions – lipoma, neuroma, angioma
Kaposi’s SA
Lymphoma
Tumors of the large intestines
Adenomas
Small to large lesions, mostly sessile
Prevalence – 20% to 30% before age 40,
40% to 50% after age 60
Most invasive colorectal adenoCA arise from preexisting
adenomatous lesion
Types- tubular, villous, tubulovillous
Malignant risk- polyp size, histologic architecture,
severity of dysplasia
-Ca is rare in tubular adenoma < 1 cm
-Ca is high (40%) in sessile villous adenoma > 4 cm
-Severe dysplasia often found in villous areas
(maximum diameter chief determinant for having cancer)
CM- small ones- asymptomatic, occult bleeding can lead to
anemia, occult bleeding – villous adenoma
All adenoma are potentially malignant
Colorectal CA
98% of all cancer in large intestines –
adenocarcinoma arise from adenomatous polyps
134,000 new cases/ year, 55,000 deaths,
15% of all cancer-related deaths USA
Epidemiology
Peak age 60-70, less than 50% seen in less than 50 y/o
if seen consider; ulcerative colitis, polyposis syndrome
Adenoma are presumed precursor lesions
Males affected 20% more often than females
Highest incidence rates in developed countries
Environmental factors- dietary practice
1.Low content of unabsorbable vegetable fiber
2.High content of refined carbohydrates
3.High fat content
4.Decrease intake vitamin A C E – increased fecal
retention, altered bacterial flora
Colorectal CA
Adenoma-carcinoma sequence- documented by these observation
3. Population with high prevalence of adenomas high prevalence of
colorectal ca
4. When invasive a is identified at an early stage surrounding
adenomatous tissue is also present
Morphology
25%- colorectal ca – cecum or ascending colon
25%- descending colon and proximal sigmoid
Tumors at Proximal colon- exophytic mass, obstruction
is uncommon Distal colon- annular encircling lesion –
napkin ring constriction
Microscopic- adenoCA well-differentiated to
undifferentiated
CM-asymptomatic and develops insidiously
R-sided- fatigue, weakness, iron deficiency anemia
L-sided- occult bleeding, change in bowel habit, crampy left lower
quadrant discomfort
Metastasis- regional LN, liver, lungs, bones
Surgically curative in 25% to 30% of cases
Most important prognostic indicator of CRC is the stage of the disease
Small intestinal neoplasms
Comprises 75% of the length of the GIT, tumor – 3% to 6% of the GIT
adenoCA- common site- duodenum
CM- late, cramping pain, N/V, weight loss
Carcinoid tumor- carcinoma-like, tendency for aggressive
behavior
6. Site of origin
7. Depth of penetration
8. Size of tumor
90% of ileal, colonic and gastric carcinoid have metastases during
time of diagnosis
can secrete bioactive products or hormones
Morphology – appendix most common site, bulbous swelling of the tip,
obliterate the lumen
Solid, yellow-tan appearance, firm due to desmoplasia
Rectal and appendiceal carcinoids almost never metastasize
Microscopic- form discrete islands, trabeculae, strands, glands or
undiffentiated sheet
Monotonous appearance with scanty pinkish cytoplasm, round to
oval stippled nuclei minimal variation in cell or nuclei size
Small intestinal neoplasms
Carcinoid syndrome- clinical features
Vasomotor disturbance (skin flushes,
cyanosis)
Intestinal hypermotility
Asthmatic attacks
Hepatomegaly (metastases)
Niacin deficiency
Systemic fibrosis
GIT- lymphoma- 40% lymphoma are
extranodal,
1% to 4% GIT cancer
Western hemisphere- arise from B-cells of
mucosa-associated lymphoid tissue (MALT)
Primary GIT lymphoma has better prognosis
Acute appendicitis
10% of people will develop AP in USA and western
countries, peak incidence in 2nd and 3rd decades
male:female ratio = 1.5:1
Pathogenesis- inflammation associated with
obstruction in 50% to 80%
Fecalith, gallstone, tumor, ball of worms (E.
vermicularis)- obstruction and ischemia
Acute appendicitis
Morphology
Early AP- dull granular red membrane
Later stage- fibrinopurulent covering at the serosa
Acute suppurative AP-
abscess formation within the wall with ulceration and
necrosis of the mucosa.
Acute gangrenous AP- green-black gangrenous
necrosis though the wall up to the serosa
Can result in rupture and suppurative peritonitis
Histologic criterion for diagnosis – neutrophilic
infitration of the muscularis propria***
Acute appendicitis
CM- classic
4.Mild periumbilical discomfort
5.Anorexia, N/V
6.RLQ tenderness
7.Deep constant ache or pain in the R
lower Q
Fever and leukocytosis appear early in the
course
Large number of cases not classic
Acute appendicitis
Differential diagnoses
3. Mesenteric lymphadenitis after viral infection
4. Gastroenteritis with mesenteric adenitis
5. PID with tubo-ovarian involvement
6. Ruptured ovarian follicle at ovulation
7. Ectopic pregnancy
8. Meckel’s diverticulitis
Mortality – appendiceal perforation = 2%
Tumors- carcinoids, mucocele non-neoplastic
obstruction of the lumen
Mucinous tumor – disseminated intraperitoneal cancer
Pseudomyxoma peritonei
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Thorax To RectumDocument35 pagesThorax To RectumdhaineyNo ratings yet
- Physical Examination of The SkinDocument3 pagesPhysical Examination of The Skindhainey100% (1)
- Anti Fungal and Anti ProtozoalDocument17 pagesAnti Fungal and Anti Protozoaldhainey100% (2)
- Anti Helminthic DrugsDocument3 pagesAnti Helminthic Drugsdhainey100% (2)
- Abdominal PainDocument12 pagesAbdominal Paindhainey100% (2)
- The Intestinal NematodesDocument9 pagesThe Intestinal NematodesdhaineyNo ratings yet
- HerniaDocument8 pagesHerniadhainey100% (1)
- Chelating AgentsDocument24 pagesChelating AgentsdhaineyNo ratings yet
- Aliphatic and Aromatic HydrocarbonsDocument13 pagesAliphatic and Aromatic HydrocarbonsdhaineyNo ratings yet
- Anti TB DrugsDocument2 pagesAnti TB DrugsdhaineyNo ratings yet
- Botanical Medications and SupplementsDocument3 pagesBotanical Medications and Supplementsdhainey100% (1)
- Cancer ChemotherapyDocument4 pagesCancer Chemotherapydhainey100% (2)
- The FilariaeDocument4 pagesThe FilariaedhaineyNo ratings yet
- TrematodesDocument5 pagesTrematodesdhaineyNo ratings yet
- Genus EchinococcusDocument6 pagesGenus EchinococcusdhaineyNo ratings yet
- Intestinal FlagellatesDocument5 pagesIntestinal Flagellatesdhainey100% (3)
- Chest and Lungs ExaminationDocument75 pagesChest and Lungs Examinationdhainey100% (10)
- Parasitology Pictures Part 2Document22 pagesParasitology Pictures Part 2dhaineyNo ratings yet
- Parasitology PicturesDocument4 pagesParasitology Picturesdhainey100% (1)
- CESTODES Intro-Pseudophyylideans-SparganosisDocument37 pagesCESTODES Intro-Pseudophyylideans-Sparganosisdhainey100% (1)
- Female Sex HormonesDocument29 pagesFemale Sex Hormonesdhainey100% (5)
- The FolateDocument3 pagesThe FolatedhaineyNo ratings yet
- Toxoplasma Pneumocystis Microsporidia BabesiaDocument40 pagesToxoplasma Pneumocystis Microsporidia BabesiadhaineyNo ratings yet
- AminoglycosidesDocument4 pagesAminoglycosidesdhaineyNo ratings yet
- Coagulants and Anti CoagulantsDocument22 pagesCoagulants and Anti Coagulantsdhainey100% (2)
- BT ReactionsDocument14 pagesBT ReactionsdhaineyNo ratings yet
- QuinolonesDocument2 pagesQuinolonesdhainey100% (1)
- Tumors of The Small and Large IntestineDocument14 pagesTumors of The Small and Large Intestinedhainey100% (4)
- Intestinal Coccidia - SarcocystisDocument29 pagesIntestinal Coccidia - Sarcocystisdhainey100% (3)
- Anti Microbial TherapyDocument39 pagesAnti Microbial Therapydhainey100% (1)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Colon CancerDocument6 pagesColon CancerUSMP FN ARCHIVOSNo ratings yet
- Anorectal DiseaseDocument122 pagesAnorectal DiseasejolagusuNo ratings yet
- A Case Study On Rectal AdenocarcinomaDocument62 pagesA Case Study On Rectal AdenocarcinomaEyySiEffVee100% (1)
- Tumors: Benign and Malignant: Cancer Therapy & OncologyDocument3 pagesTumors: Benign and Malignant: Cancer Therapy & OncologyMaria ArifahNo ratings yet
- Phytochemical Analysis in Capsicum SPP.: March 2016Document154 pagesPhytochemical Analysis in Capsicum SPP.: March 2016AbdurrohimnNo ratings yet
- Pathophysiology of Colon CancerDocument3 pagesPathophysiology of Colon CancerJaymica Laggui DacquilNo ratings yet
- Oncology Nursing HandoutsDocument7 pagesOncology Nursing HandoutsShandz de Rosas100% (1)
- Ijmm 31 6 1375 PDFDocument6 pagesIjmm 31 6 1375 PDFAlex RogobeteNo ratings yet
- Colorectal Cancer - Epidemiology, Risk Factors, and Protective Factors - UpToDateDocument38 pagesColorectal Cancer - Epidemiology, Risk Factors, and Protective Factors - UpToDateYdeli DetanNo ratings yet
- Prevention & Detection of CANCERDocument32 pagesPrevention & Detection of CANCERSiddharth JainNo ratings yet
- Exercise For Cancer PatientsDocument1 pageExercise For Cancer PatientsAdvanced PhysiotherapyNo ratings yet
- Exercise As Defensive Nutritional Paradigm - MSC Sem3FPP - 19-20 - NALSDocument18 pagesExercise As Defensive Nutritional Paradigm - MSC Sem3FPP - 19-20 - NALSdrashti shahNo ratings yet
- Surgery Oral Exam CASES JMC 12 2008 V2Document17 pagesSurgery Oral Exam CASES JMC 12 2008 V2aaronlhuangNo ratings yet
- Factors Associated With Short-Term Mortality After Surgical Oncologic EmergenciesDocument12 pagesFactors Associated With Short-Term Mortality After Surgical Oncologic EmergenciesErinda SafitriNo ratings yet
- Diet IBS PDFDocument31 pagesDiet IBS PDFIesanu MaraNo ratings yet
- UntitledDocument20 pagesUntitledstuffednurseNo ratings yet
- Colorectal Cancer Screening Risk Factors and StatisticsDocument2 pagesColorectal Cancer Screening Risk Factors and StatisticsFarasha SSNo ratings yet
- Practice Guidelines For Tumor Marker Use in The Clinic: Catharine SturgeonDocument9 pagesPractice Guidelines For Tumor Marker Use in The Clinic: Catharine SturgeonYder AtrupNo ratings yet
- CRCDocument5 pagesCRCanon_619577898No ratings yet
- ColonosDocument20 pagesColonosshaneatateNo ratings yet
- CancerDocument84 pagesCancerKaruna KumariNo ratings yet
- 2007 MLH1Document6 pages2007 MLH1Mericia Guadalupe Sandoval ChavezNo ratings yet
- Colorectal CancerDocument8 pagesColorectal Cancerjorgeacct100% (3)
- Cancer-Surviving Against The Odds - Brian CoxDocument58 pagesCancer-Surviving Against The Odds - Brian CoxwobblegobbleNo ratings yet
- Wife Misses Intimacy: Tomorrow's HoroscopeDocument1 pageWife Misses Intimacy: Tomorrow's HoroscopeThe Delphos HeraldNo ratings yet
- Colon: Colorectal Cancer, Also Called Colon Cancer or Large Bowel Cancer, IncludesDocument6 pagesColon: Colorectal Cancer, Also Called Colon Cancer or Large Bowel Cancer, IncludesMhackie Perez100% (1)
- Diagnosis NeoplasiaDocument23 pagesDiagnosis NeoplasiaRatuNadiaMaharani100% (1)
- 1.04 Large Intestine, Colon, and RectumDocument15 pages1.04 Large Intestine, Colon, and RectumZazaNo ratings yet
- Capsules DR Mohammed EidDocument246 pagesCapsules DR Mohammed EidMohammad BanisalmanNo ratings yet
- Intestinal Obstruction, Colorectal CancerDocument49 pagesIntestinal Obstruction, Colorectal CancermeghanaNo ratings yet